COVID-19 How many Healthcare workers are infected?
April 17, 2020
Carl Heneghan, Jason Oke, Tom Jefferson
The UK government holds a daily briefing and releases data on new UK COVID 19 cases.
In the assessment of new UK cases, the Gov’t defines Pillar 1 cases as NHS Medical need and most critical key workers; Pillar 2 is those who undergo commercial-swab testing for critical key workers in the NHS and other sectors.
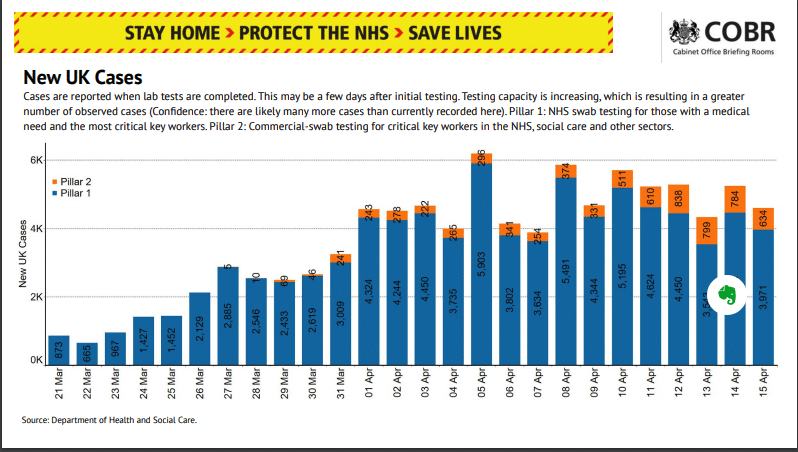
Here’s the 15th April cabinet briefing; and the Slides and datasets to accompany the 16th April meeting
Data from the 15th show that 13.8% of positives are critical key workers in the NHS and other sectors. Data from the 16th April shows 16.2% are critical key workers.
Using Poisson regression model for count data, and not including the first four data points of pillar 2 due to them being non-linear, we observe that the Pillar 1 rate increased at a rate of 2.0 % per day, while the Pillar 2 rate increased at a faster rate of 9.1% per day (this is a conservative estimate as including the early data increases the pillar 2 rate).
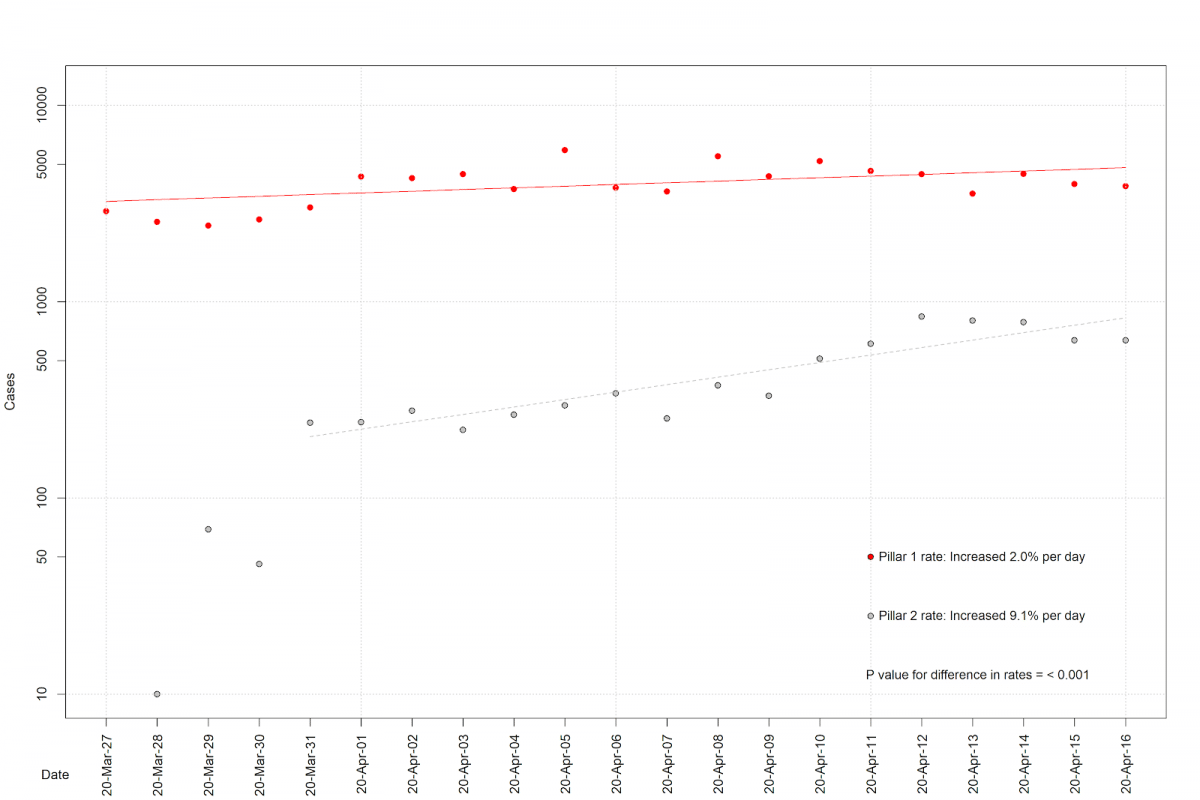
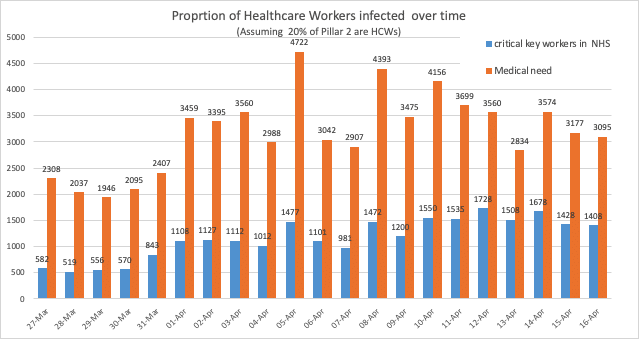
To work out the HCW related infection rates overall is difficult. As they seem to be in both PIllar 1 and 2 counts (Pillar 1 includes the most critical key workers).
If we assume that 20% of the Pillar 1 ‘critical key workers’ are HCW related, then we can estimate that nearly a third (1408/4618 = 30.5%) of all infected cases on the 16th of April are related to HCWs.
In our article on the Tipping Point, we highlighted that in Italy over-referral led to significant numbers of unwell people turning up or sent into hospital in Lombardy. The disease then spread rapidly in the hospital setting. Healthcare workers then had a higher risk of exposure and became vectors of onwards transmission. In China, more than 3,300 healthcare workers were infected (4% of the 81,285 reported infections). In Spain on the 25th March, nearly 6,500 medical personnel were infected (13.6%) of the country’s 47,600 total cases – 1% of the health system’s workforce.
In the way out of this pandemic, we pointed out that HCW infection was a big problem in the SARS 2002-03 outbreak in Toronto, as onward transmission occurred mainly within health care settings. A retrospective analysis of 138 patients In Wuhan support this as the hospital-associated transmission was suspected in 41% of the cases.
The proportion of HCWs in Pillar 1 may be higher, or lower than our estimate. We cannot tell. Anecdotal evidence supports a larger number of HCWs are being infected: in Newport, Wales, about half the emergency department team have tested positive. However, without comprehensive testing of HCWs, we will never really know how are infected.
Reducing transmission in hospitals and amongst HCWs remains vital to resolving this outbreak.
AUTHORS
Carl Heneghan is Professor of Evidence-Based Medicine, Director of the Centre for Evidence-Based Medicine and Director of Studies for the Evidence-Based Health Care Programme. (Full bio and disclosure statement here)
Jason Oke is a Senior Statistician at the Nuffield Department of Primary Care Health Sciences and Module Coordinator for Statistical Computing with R and Stata (EBHC Med Stats), and Introduction to Statistics for Health Care Research (EBHC), as part of the Evidence-Based Health Care Programme.
Tom Jefferson is an Epidemiologist. Disclosure statement is here

