How can pandemic spreads be contained in care homes?
April 14, 2020

Mona Koshkouei, Lucy Abel and Caitlin Pilbeam
On behalf of the Oxford COVID-19 Evidence Service Team
Centre for Evidence-Based Medicine
Nuffield Department of Primary Care Health Sciences
University of Oxford
How can pandemic spreads be contained in care homes? Taking into account:
1. Human resources
2. Nursing activities/medications
3. The role of external visitors
VERDICT
Effectiveness of infection control measures is dependent upon a number of factors and a combination of strategies with the most significant being:
– Hand hygiene – Access to hand hygiene facilities at the workspace, in addition to use of four or more of the WHO multi-modal strategy generally improve adherence to hand hygiene measures
– Environmental decontamination – Daily cleaning of most touched surfaces and weekly deep clean
– Staff rotation – Allocating staff to one facility consistently may reduce spread across several locations
– Visitors – Restricting visitation to only emergency/critical cases
– Testing – Creates rapid response in placing added measures to contain and prevent further spread
BACKGROUND
Care home settings serve a primarily elderly population with a diverse range of medical requirements. Care homes are unique in being both health-related institutions and people’s home (1) (2). In available data the risk of dying from COVID-19 increases with age, and most of the deaths observed are in people older than 60 (3). Studies of care home residents have shown that respiratory tract infection (RTIs) outbreaks are more frequent than gastrointestinal and spread more quickly amongst the population, with less autonomous residents being more severely affected by RTIs such as influenza (4).
Introducing further complexity, residents may have diverse needs through health and functional status, potentially exhibiting behaviours that compromise infection control (e.g. spitting), carers vary in levels of training, and facilities themselves differ in how they are set up and run.
In response to the COVID-19 pandemic many such settings have introduced restrictions on visitors to minimise the risk of spreading the infection to their residents. This rapid review evaluates available measures to minimise the risk of infection spread among residents and staff within care home settings.
SEARCH STRATEGY
Two searches were conducted. One aimed to identify studies relating to viral infection control in care homes, while the second aimed to identify studies pertaining to pandemic responses in care homes. Searches were conducted on PubMed.
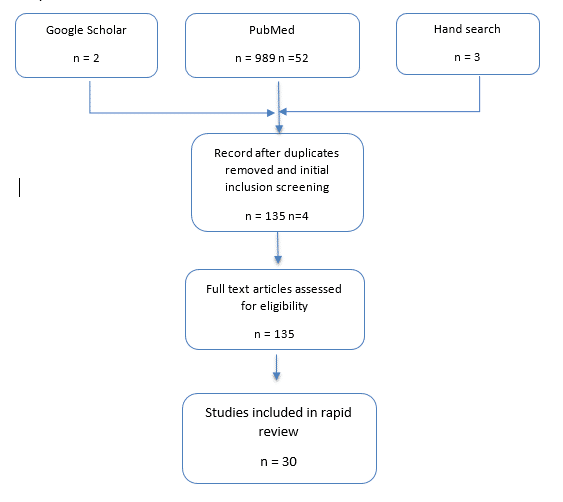
Inclusion:
1. Trials, observational studies, systematic reviews, database studies, policy papers, guidelines, working papers, Government document, Guidelines, Legislation, Practice guidelines
2. Respiratory including influenza, gastrointestinal and viral infections including norovirus
Exclusion:
1. Animal studies
2. Papers not in English or Persian
3. Opinion pieces
4. Schools, childcare and paediatric facilities
5. Antibiotic resistance studies
6. Influenza and pneumococcal vaccine studies
7. Disease/conditions: UTI, Clostridium difficile, scabies, general bacterial infections
8. No abstract or full text availability
Search terms:
Search 1 (((((facilities, residential[MeSH Terms]) OR(care home*[Text Word] OR nursing home*[Text Word] OR residential home*[Text Word] OR group home*[Text Word])) AND ((infection control[MeSH Terms]) OR (infection control[Text Word] OR disinfect*[Text Word])))) OR (((coronavirus*[Title] OR coronovirus*[Title] OR coronoravirus*[Title] OR coronaravirus*[Title] OR corono-virus*[Title] OR corona-virus*[Title] OR “Coronavirus”[Mesh] OR “Coronavirus Infections”[Mesh] OR “Wuhan coronavirus” [Supplementary Concept] OR “Severe Acute Respiratory Syndrome Coronavirus 2″[Supplementary Concept] OR COVID-19[All Fields] OR CORVID-19[All Fields] OR “2019nCoV”[All Fields] OR “2019-nCoV”[All Fields] OR WN-CoV[All Fields] OR nCoV[All Fields] OR “SARS-CoV-2”[All Fields] OR HCoV-19[All Fields] OR “novel coronavirus”[All Fields])) AND ((facilities, residential[MeSH Terms]) OR(care home*[Text Word] OR nursing home*[Text Word] OR residential home*[Text Word] OR group home*[Text Word]))))
Filters: Humans
Search 2 ((((((facilities, residential[MeSH Terms]) OR care home[Title/Abstract]) OR nursing home[Title/Abstract]) OR residential care[Title/Abstract]))) AND ((((((“pandemics”[MeSH Terms] OR “pandemics”[All Fields] OR “pandemic”[All Fields]) OR (“coronavirus”[MeSH Terms] OR “coronavirus”[All Fields])))))
QUALITY ASSESSMENT
Quality assessment was conducted informally. Papers were evaluated based on study design, but due to the lack of relevant papers, selection was predominantly based on relevance of population, intervention, and condition. Discussion of inclusion and exclusion of studies took place between all three researchers.
The majority of studies relating to outbreak management in care homes assumed an influenza outbreak with a vaccine available. Evidence relating to management in the absence of a vaccine was sparse.
SUMMARY of findings from most useful papers
A number of prevention measures have been employed in care home settings globally. A summary of potential interventions and their effectiveness is described under the five key headings below.
Hand hygiene
The effectiveness of hand hygiene for preventing spread of infection is well documented, and a number of papers evaluated interventions to improve hand hygiene among staff in care homes. These were of mixed quality, often using a before-and-after study design without a control group. Infection control interventions focussing on education generally showed mixed or negative results (5, 6). Cohort studies that evaluated care home characteristics similarly did not find a relationship between infection control training programmes and outbreaks (7, 8).
A mixed-method study analysing nursing staff’s behaviour and knowledge towards hand hygiene found that whilst most hand hygiene equipment was readily available, compliance to these infection control measures depended upon the equipment’s immediate availability in the work area and line manager’s compliance to the measures. The use of gloves was seen by some as an effective measure and thus resulted in an increased incidence of hand hygiene upon their removal (1). Another common barrier was reported as skin sensitivity or damage (9).
An effect has been demonstrated in the use of hand sanitiser. One cluster RCT evaluated an intervention that combined education and reminders, with each staff member being given a pocket-sized hand sanitiser. This was found to be effective in improving compliance, reducing pneumonia infection, and reducing infection deaths (10). Likewise, a case-control study of hand sanitiser being made available also found a reduction in infection rates (11).
A systematic review assessing five studies, including three cluster randomised trials, demonstrated that the use of four or more of the WHO multi-modal strategy (12) were generally associated with decreased respiratory infections, and resulted in improved adherence to hand hygiene measures. The same review found evidence that a combination of education, monitoring, and feedback provided the most effective measure in driving behavioural change in healthcare workers to implement and maintain infection control strategies (13).
Key point: While education interventions to improve hand hygiene in care homes achieve limited results, adequate provision of hand sanitiser and gloves, along with line management support, have been shown to reduce infection rates.
Environmental decontamination
The spread and transmission of COVID-19 is now well documented in literature with an estimated life expectancy on a variety of surfaces. A before-and-after study in an American nursing home using Ultraviolet light in assisting disinfection processes found that weekly use of a pulsed-xenon disinfection device, in additional to daily manual disinfecting, reduced respiratory system infection rates and hospitalization by pneumonia (14). It is unclear if this is due to the effects of UV light on, including photocrosslinking resulting in viral death, or bias introduced through more thorough manual cleaning by staff.
Key point: Regular disinfection of high-traffic surfaces reduces infection spread. Disinfection devices may support this.
Staffing
Cohort studies and simulations that modelled care home characteristics found that larger care homes were at greater risk of pandemic outbreaks than smaller ones. These studies also found that staff were a key source of outbreaks and transmission; in particular, staff entry and re-entry, including community nurses working across a number of locations (7, 15).
A number of surveys have been conducted on pandemic preparedness, one specifically for the UK context (16). This study reported that UK care homes expected to be reliant on temporary “bank” staff as their own staff took sick leave. This may leave care homes particularly vulnerable.
Key point: The evidence supports limiting movement of staff between care homes. Care homes relying on temporary staff should be aware that these staff are a key potential source of infection.
Visitors
We did not find any evidence specifically on the effectiveness of preventing or limiting visitors to the care home. However, as staff movement is a risk factor for outbreaks, so similarly may visitors be a potential source of infection during a pandemic with widespread community transmission.
Key point: No evidence on restricting visitors was identified, but if visitors have similar impact as staff re-entry, then restriction is supported.
Testing
Evidence exists that prompt identification of an outbreak, typically less than three days (8), is required for providers to coordinate an effective response, in addition to routine/standard infection control precautions. Such measures include introduction of contact and droplet precautions such as PPE, isolating cases, and cancelling group activities and meals (17).
We did not identify any evidence on testing strategies for staff, although staff testing may be effective in limiting outbreaks given the evidence on staffing discussed above.
Key point: Rapid identification of cases among both staff and residents through testing may facilitate a coordinated response that minimises within-care home spread, although further evidence is needed.
Resident wellbeing
Holistic wellbeing in care homes is also an important consideration. Whilst there is some acknowledgement of the potential impact of different public health measures and emergencies on care home residents and their families, this area is under-researched.
Particular concerns expressed in literature include that physical isolation practices, suspension of visiting hours and care home activities, and restrictions on movement within the facility may increase loneliness and depressive feelings. For dementing patients, for example, regular interaction with familiar staff brings comfort, but staff wearing face-masks may be scary or confusing (18). There is also potential worry about and fear of health threats in care home residents, who may feel and be particularly vulnerable, or may not know very much about the public health emergency (19).
One study reviewed the perspective of care home residents in Hong Kong during the SARS epidemic (19). This study emphasised the participation of residents in reducing the risk of spread and recommended an education programme for residents, both to encourage buy-in to mitigation practices, and to address fears and safeguard residents’ quality of life.
Key point: Quality of life is an important consideration when planning responses to public health emergencies in care homes. Education of residents can aid compliance with mitigation strategies, and address considerations of quality of life and anxiety. Further research on maintaining quality of life in care homes during outbreaks is urgently needed.
Implementation challenges
Challenges in implementing infection control guidance during outbreaks was variable and included: maintaining adequate staffing; maintaining supplies necessary for implementation of infection control precautions; the potential negative impacts of restricting residents to their rooms; and difficulties controlling the movement of residents with dementia (17).
Case isolation
Recommendations from Public Health England have included advice to isolate symptomatic patients. We did not identify any evidence on the effectiveness of this for viral infections in care homes.
Coronavirus case study
The only study yet published on COVID-19 in care homes (21) is a report of the spread of an outbreak through an American care home, finding that the virus spread quickly among the majority of residents, staff, and visitors, with 81 cases among the approximately 130 residents.
The authors identified the following factors that contributed to the outbreak:
• staff continuing to work while symptomatic;
• staff members working in more than one facility;
• inadequate adherence to standard droplet and contact precautions, and eye protection recommendations;
• poor infection control practices due, in part, to inadequate supplies of personal protective equipment and hand sanitiser;
• delayed recognition of cases, limited testing availability, and difficulty identifying COVID-19 cases based on signs and symptoms alone.
These factors, although from a single site, closely match the findings of the available literature.
References
1. Hammerschmidt J, Manser T. Nurses’ knowledge, behaviour and compliance concerning hand hygiene in nursing homes: a cross-sectional mixed-methods study. BMC Health Serv Res. 2019;19(1):547.
2. Nicolle LE. Preventing infections in non-hospital settings: long-term care. Emerg Infect Dis. 2001;7(2):205-7.
3. Lloyd-Sherlock P, Ebrahim S, Geffen L, McKee M. Bearing the brunt of covid-19: older people in low and middle income countries. Bmj. 2020;368:m1052.
4. Gaspard P, Mosnier A, Simon L, Ali-Brandmeyer O, Rabaud C, Larocca S, et al. Gastroenteritis and respiratory infection outbreaks in French nursing homes from 2007 to 2018: Morbidity and all-cause lethality according to the individual characteristics of residents. PLoS One. 2019;14(9):e0222321.
5. Eveillard M, Raymond F, Guilloteau V, Pradelle MT, Kempf M, Zilli-Dewaele M, et al. Impact of a multi-faceted training intervention on the improvement of hand hygiene and gloving practices in four healthcare settings including nursing homes, acute-care geriatric wards and physical rehabilitation units. J Clin Nurs. 2011;20(19-20):2744-51.
6. Gopal Rao G, Jeanes A, Russell H, Wilson D, Atere-Roberts E, O’Sullivan D, et al. Effectiveness of short-term, enhanced, infection control support in improving compliance with infection control guidelines and practice in nursing homes: a cluster randomized trial. Epidemiol Infect. 2009;137(10):1465-71.
7. Lin H, Ng S, Chan S, Chan WM, Lee KC, Ho SC, et al. Institutional risk factors for norovirus outbreaks in Hong Kong elderly homes: a retrospective cohort study. BMC Public Health. 2011;11:297.
8. Friesema IH, Vennema H, Heijne JC, de Jager CM, Morroy G, van den Kerkhof JH, et al. Norovirus outbreaks in nursing homes: the evaluation of infection control measures. Epidemiol Infect. 2009;137(12):1722-33.
9. Kingston LM, Slevin BL, O’Connell NH, Dunne CP. Hand hygiene: Attitudes and practices of nurses, a comparison between 2007 and 2015. Am J Infect Control. 2017;45(12):1300-7.
10. Yeung WK, Tam WS, Wong TW. Clustered randomized controlled trial of a hand hygiene intervention involving pocket-sized containers of alcohol-based hand rub for the control of infections in long-term care facilities. Infect Control Hosp Epidemiol. 2011;32(1):67-76.
11. Fendler EJ, Ali Y, Hammond BS, Lyons MK, Kelley MB, Vowell NA. The impact of alcohol hand sanitizer use on infection rates in an extended care facility. Am J Infect Control. 2002;30(4):226-33.
12. Organization WH. Summary of the multi modal strategy 2007 [Available from: https://www.who.int/gpsc/news/simple_guideline/en/.
13. Lee MH, Lee GA, Lee SH, Park YH. Effectiveness and core components of infection prevention and control programmes in long-term care facilities: a systematic review. J Hosp Infect. 2019;102(4):377-93.
14. Kovach CR, Taneli Y, Neiman T, Dyer EM, Arzaga AJ, Kelber ST. Evaluation of an ultraviolet room disinfection protocol to decrease nursing home microbial burden, infection and hospitalization rates. BMC Infect Dis. 2017;17(1):186.
15. Nuño M, Reichert TA, Chowell G, Gumel AB. Protecting residential care facilities from pandemic influenza. Proceedings of the National Academy of Sciences. 2008;105(30):10625.
16. Fell G. Preparedness of Residential and Nursing Homes for Pandemic Flu. Journal of Public Health. 2008;30(1):99-102.
17. Pena SA, Davis SS, Lu X, Sakthivel SKK, Peret TCT, Rose EB, et al. Severe Respiratory Illness Associated with Human Metapneumovirus in Nursing Home, New Mexico, USA. Emerg Infect Dis. 2019;25(2):383-4.
18. Sitoh YY. Severe acute respiratory syndrome: effect on community and residential aged care services in Singapore. J Am Geriatr Soc. 51. United States2003. p. 1505-6.
19. Tse MM, Pun SP, Benzie IF. Experiencing SARS: perspectives of the elderly residents and health care professionals in a Hong Kong nursing home. Geriatr Nurs. 2003;24(5):266-9.
20. Jackson MM, Lynch P. An alternative to isolating patients. Geriatr Nurs. 1987;8(6):308-11.
21. McMichael TM, Currie DW, Clark S, Pogosjans S, Kay M, Schwartz NG, et al. Epidemiology of Covid-19 in a Long-Term Care Facility in King County, Washington. N Engl J Med. 2020.
Competing interests: No competing interests
Disclaimer: The article has not been peer-reviewed; it should not replace individual clinical judgement and the sources cited should be checked. The views expressed in this commentary represent the views of the authors and not necessarily those of the host institution, the NHS, the NIHR, or the Department of Health and Social Care. The views are not a substitute for professional medical advice.
About the authors
Mona Koshkouei is a Pharmacist and DPhil researcher in the Nuffield Department of Primary Care Health Sciences, University of Oxford and Pharmacist Teaching Fellow at Kingston University London.
Lucy Abel is a Health Economist and DPhil researcher in the Nuffield Department of Primary Care Health Sciences, University of Oxford.
Dr Caitlin Pilbeam is a Medical Anthropologist who is a postdoctoral researcher in global health and tutor in qualitative research methods in the Nuffield Department of Primary Care Health Sciences, University of Oxford.

