PCR positives: what do they mean?
September 17, 2020
Updated 23 September 2020
Article by:
info@future-synthesis.com
fsdataanalysis@gmail.com
matteo.chiesa@uit.no
sergio.s.hernandez@uit.no
Department of Physics and Technology, UiT The Artic University of Norway
9037 Tromsø, Norway, Future Synthesis AS Uniongata 18, 3732 Skien, Norway
PCR positives: what do they mean?
Download Pdf: PCR test REFERENCE_Infectivity 2020 Nov 5
Watch video: False Positives and Rapid Tests Explained
Contents
- Is the PCR test sensitive enough?. page 2
- Culturing a virus as reference test page 2
- Does a PCR “TRUE POSITIVE” mean INFECTIVITY OR VIRULENCE?. page 2
- PCR true positives versus infectivity and virulence. page 3
- Explanation of the experiment that shows whether a virus is still infective. page 4
- Is there evidence that someone is infectious after PCR results?. page 4
- Can successive tests on the same person give contradictory results?. page 5
- How long can an inactive virus remain in a body? page 5
- PCR kits for SARS Cov2 (manufacturers and asymptomatic) page 6
- Conclusion in relation to PCR positives and an advancing pandemic. page 6
- Are PCR tests helpful?. page 7
- Statistical analysis: PCR positives and deaths (excess deaths) page 7
- CONCLUSIONS. page 9
Is the PCR test sensitive enough?
The PCR is very sensitive and will detect the presence of viral RNA (with PCR the virus is detected by targeting one or more gene fragments). The gene fragment might be detected and the virus “positively found”. But is this viral RNA active? That is, does the detected viral RNA have the capacity to reproduce or infect the person (virulence) or get transmitted to other people (infectivity)?
The Centre for Evidence-Based Medicine (CEBM) says[1, 2]:
“PCR detection of viruses is helpful so long as its accuracy can be understood: it offers the capacity to detect RNA in minute quantities, but whether that RNA represents infectious virus may not be clear.”
Culturing a virus as reference test
What are a reference test and a baseline? Many experiments in science are relative in the sense that they do not give absolute values or need to account for context dependent data. In this sense, it is typical of scientific instrumentation and measurements to require calibration or a baseline. The baseline and calibration allow the scientist to interpret the results. In this respect, the CEBM writes:
“Viral culture [acts] as reference test against which any diagnostic index test for viruses must be measured and calibrated, to understand the predictive properties of that test.”
Does a PCR “TRUE POSITIVE” mean INFECTIVITY OR VIRULENCE?
What does viral culture tell about PCR positives?
A PCR test might find the virus it was looking for. This results in a PCR positive, but a crucial question remains: is this virus active, i.e. infectious, or virulent? The PCR alone cannot answer this question. The CEBM explains why culturing the virus is needed to answer this question:
“In viral culture, viruses are injected in the laboratory cell lines to see if they cause cell damage and death, thus releasing a whole set of new viruses that can go on to infect other cells.”
That is, if the PCR detects the virus in the human sample, this detection might correspond to a virus that is now incapable of infecting cells and reproducing. Biologists can tell if the virus is infectious by injecting it into cells (culture cells). If these cells are not affected by the virus and the virus does not reproduce in them, then the PCR test found a virus that is no longer active.
The meaning is that the PCR positive is a non-infectious positive.
PCR true positives versus infectivity and virulence
Does a PCR positive mean TRUE POSITIVE if the gene fragments targeted in the PCR are unique to the virus and the PCR is VERY ROBUST?
There is speculation as to whether the PCR can indeed find the virus from a person’s sample or maybe the PCR is not specific enough and might give positive when other viruses are present. Some PCR manufacturers tell us there is “cross contamination” and “non-specific” interference with a list of viruses and other in their instructions manuals[3, 4].
POSSIBILITY ONE: the PCR test is positive, but this was due to cross-contamination or non-specific interactions. Then the test would be a FALSE POSITIVE because the SARS Cov2 virus is not present in the sample. This means the PCR positive is a FALSE POSITIVE rather than a TRUE POSITIVE. But this is not the only possibility. We want to focus on the CEBM argument that depends on viral culture.
POSSIBILITY TWO: Even if the PCR test only detects TRUE POSITIVES in the sense that the SARS Cov2 virus, or better, the target gene fragment, is present in the sample, it remains to be seen whether the person can infect others or even if the virus is still infecting the very person carrying the virus.
What did Tom Jefferson et al. find in their investigation regarding viral culture of SARS Cov2 in order to assess infectivity (horizontal transmission or capacity for a virus to spreads among hosts) and virulence (a pathogen’s ability to infect or damage a host):
“We, therefore, reviewed the evidence from studies reporting data on viral culture or isolation as well as reverse transcriptase-polymerase chain reaction (RT-PCR), to understand more about how the PCR results reflect infectivity.”
What does this mean? The authors wanted to find out if 1) PCR TRUE POSITIVE meant that the virus found in the person could be transmitted to other people or was virulent or 2) the virus was no longer infective or virulent.
Explanation of the experiment that shows whether a virus is still infective
Imagine that a virus enters your body. In a few months it might not do anything to you anymore. It might not do anything to your cells (virulence), and it might also lack the capacity to move into another person (infectivity) when you speak or sneeze. It is also possible that this virus simply never did anything to you and lacked infectivity from the very beginning. But traces of the virus might still be present in the person. In this case, the virus is present but inactive.
So how do you know if the virus is active? You do the PCR. If the virus is found in the person (PCR TRUE POSITIVE), that virus is injected into a culture cell. If by injecting that virus into culture cells, the virus is not able to reproduce in the cells, that virus cannot infect anybody any longer. This means that even if you are a PCR positive, you are no longer contagious, that is, the virus in you is no longer active.
Conclusion: A TRUE POSITIVE in PCR does not always mean that the person presents any danger to society. The virus cannot be transmitted when cell culture shows that the virus is not infective. Unfortunately relating PCR POSITIVE to infectivity is not easy if we consider the whole population. This would need 1) a model (correlation) that maps PCR POSITIVES and/or symptoms to infectivity as tested by viral culture or 2) viral culture for every individual case. See next.
Is there evidence that someone is infectious after PCR results?
Tom Jefferson et al. claim that after searching for the PCR to viral culture correlation no conclusion was found since time from collection and symptoms severity are needed for the correlation amongst other to find an appropriate model. We recall that currently they (governments) hardly look for symptoms in people. Positives are called PCR Positive asymptomatic if they present no symptoms. In the article the authors say:
“Data are sparse on how the PCR results relate to viral culture results. There is some evidence of a relationship between the time from collection of a specimen to test, symptom severity and the chances that someone is infectious.
One of the studies we found (Bullard et al) investigated viral culture in samples from a group of patients and compared the results with PCR testing data and time of their symptom onset.” Figure 1.
Conclusion:
“It was not possible to make a precise quantitative assessment of the association between RT-PCR results and the success rate of viral culture within these studies.
This means that PCR Positives might or might not lead to concluding that a subject testing positive by PCR is infectious. Why? Because PCR positives have not been correlated to the growth of the virus in culture. They continue to explain why this correlation is not possible:
“These studies were not adequately sized nor performed in a sufficiently standardised manner and may be subject to reporting bias.”
Can successive tests on the same person give contradictory results?
That a PCR test gives positive or negative depends on how the experiment is conducted. Furthermore, since it is not known whether and how PCR positives correlates to infectivity and how it is that this correlation must be interpreted, the interpretation of a PCR POSITIVE is inconclusive. The authors claim:
“Cycle thresholds are the times that the amplifying test has to be repeated to get a positive result. The higher the viral concentration the lower amplification cycles are necessary.”
Some people might give positive after running the PCR test with a high threshold and others with a low threshold. The threshold alone might or might not tell whether someone carries infective viral RNA.
How long can an inactive virus remain in a body?
This is inconclusive since PCR positives to viral culture studies are lacking and cycle thresholds should also be considered. See above. The way in which the experiment is carried out however, matters. This is because one might be PCR Positive long after the virus is no longer active. The authors briefly explain why:
“This detection problem is ubiquitous for RNA virus’s detection. SARS-CoV, MERS, Influenza Ebola and Zika viral RNA can be detected long after the disappearance of the infectious virus. … because inactivated RNA degrades slowly over time it may still be detected many weeks after infectiousness has dissipated.”
The authors show a figure (figure 2) where it is noted that the presence and detection of viral RNA by PCR does not imply that the virus is infectious or virulent any longer.
PCR kits for SARS Cov2 (manufacturers and asymptomatic)
PCR positives on asymptomatic people should be treated with care since it is possible that the asymptomatic people are not infectious. This is even when the PCR tests or the antibody tests are positive. This is because viral culture is required to establish if the viral RNA is capable of infecting cells and “reproduce”.
PCR manufacturers typically remind the users that “the detection result of this product is only for clinical reference, and it should not be used as the only evidence for clinical diagnosis and treatment[3]” and “designed for the specific identification and differentiation of the new coronavirus (SARS-CoV-2) in clinical samples from patients with signs and symptoms of Covid19”.
Conclusion in relation to PCR positives and an advancing pandemic
Conclusion: symptoms and signs of Covid19 are necessary to support the claim that the subject is or can be infectious. But calling PCR positives “cases” does not specify whether the persons have carried the virus for long or whether it is “active”. This could lead to the finding of many “cases” as a function of the number of PCR tests conducted. For example, if 20% of a population are PCR positive, the number of PCR positives will depend on the size of the sample. This means that the more PCR test are carried out the larger the fraction of the population that is confirmed but this might not speak of changes in the population. That is, it is possible that the population was infected already long before deciding to test and PCR positives would therefore not speak of “an advancing pandemic”
Are PCR tests helpful?
It is typical now to call PCR positives that present no symptoms asymptomatic (see above). It is highly likely that these tests are detecting viral RNA in patients where the virus is no longer capable of infecting. A statistical test where biological equipment would not be required could involve correlating deaths to PCR positives (we discuss this next )The CEBM authors claim:
“PCR detection of viruses is helpful so long as its limitations are understood; while it detects RNA in minute quantities, caution needs to be applied to the results as it often does not detect infectious virus.”
Statistical analysis: PCR positives and deaths (excess deaths
We start by claiming that if PCR positives have any predictive power on the number of deaths expected, there should be some correlation, i.e. the more PCR positives (SARS Cov2) today the more deaths by Covid19 in the future (at least a few days later but presumably 2-4 weeks later at least if the PCR is taken just after infection). Figure 3 illustrates this.
However, in figure 4 we show PCR positives versus Covid19 deaths as labelled by the Spanish ministry of health. https://www.mscbs.gob.es/profesionales/saludPublica/ccayes/alertasActual/nCov/documentos/Actualizacion_207_COVID-19.pdf
Covid19 labelled death versus TRUE death by Covid19
We differentiate between labelled Covid19 and death by Covid19 as the true cause of death. Since we cannot know the true cause of death (this is done by medical examiners but the results are or can be relatively subjective) we will also discuss excess deaths later. A ratio between infections and deaths is the typical way in which mortality is considered[5]. A simple function between PCR positives to Covid19 could be a linear function (Eq. 1). We can add a time delay indicating that it takes time for people to die after being infected (Figures 3 and 4). This function should have some predictive power to be useful. If so, there should be correlation. Here D(t) is the number of deaths at time t (or a given day) and P(t*) is the number of PCR positives at an earlier time t*=t-t0, where t0 is the time between the number of deaths D recorded and the number of PCR Positives recorded (typically days to weeks as shown in Figure 5). Here α is the effective mortality rate, i.e. for a number of PCR Positives P, D deaths should be expected after a t0 (α =D/P).

Figure 5 shows schematically that t0 is expected to be between 20 and 30 days roughly (4 weeks) and on average. Ideally and accordingly, if the PCR tests were performed during the very first days of infection, Eq. 1 would give us some predictive power over the number of deaths by Covid19 expected in t0 days (time).
For the Spanish data (Figures 4, 6 and 7) the key points are:
- Figure 4 shows that the same order of magnitude of positives was recorded in March-April 2020 as in July-August-September 2020 but the number of deaths was much lower in August to September (data from the Spanish Ministry of Health). This means that 1) either we do not have the true infection fatality ratio (IFR) but a (CFR), 3) the cases in March-April correspond to different phenomena to those in July-September, or 3) the virus has mutated so rapidly that the true IFR has changed already and dramatically. We believe that the second point here is key and the explanation is that the cases in March-April were cases of truly infected people whereas in July-September the cases correspond to people that have mostly passed the infection already, i.e. will not die. The confirmation of this hypothesis would be given by viral culture experiments as discussed by Jefferson et al. above.
- Figure 6 shows that the peak in PCR positives in March-April does not lead to a peak in deaths at the end of April. We ran a correlation test and got numbers in the 0.4-0.2 range. If a delay of 10-20 days is allowed, implying that we want to predict deaths in the future from PCR positives today, the correlation coefficient gave us numbers below 0.2 (not shown). The same happens with the more decent data in July August (not shown).
What if we take into account excess deaths instead?
The data for total deaths in 2020 in Spain, mean number of deaths for the years 2010 to 2019 and confidence interval for those years is provided by the Spanish Ministerio de Ciencia e Innovación at https://www.isciii.es/QueHacemos/Servicios/VigilanciaSaludPublicaRENAVE/EnfermedadesTransmisibles/MoMo/Paginas/Informes-MoMo-2020.aspx)
We might argue that labelled deaths are not in agreement with the true number of deaths by Covid19. If we take excess deaths instead, this being the number of deaths in 2020 compared to previous years (2010-2019) we can plot the normalised excess deaths (blue) against normalised PCR positives (black) in Figure 7. There is no time delay between PCR tests and excess deaths as shown in Figure 7 and it could be argued that this could explain the lack of correlation. We applied a time delay and checked the coefficient of determination for delays ranging from 0 to 45 days (Figure 8).
The highest value for the coefficient of determination R2 was found by applying no delay as seen in Figure 8. The implication is that the number of positive PCR cases is proportional to the excess deaths reported that day, i.e. with no time delay. If that was the case the PCR testing would be ultimately redundant since knowing the excess deaths tells you at once excess deaths that day which is the variable targeted in the study. We still find no meaningful correlation (correlation coefficients still much below 0.5, Figure 8) by applying delays as shown in Figure 8. Data from May to the end of August is shown in a scatter diagram, i.e. PCR positives versus excess deaths, in Figure 9.
CONCLUSIONS
As shown in Figure 8, the more delay we give to the PCR positives recorded on a given day in relation to the excess deaths recorded, the lower R2. A delay of at least a few days to weeks would be meaningful, i.e. would imply PCR positives predict the number of deaths in the future since governments could “expect” what is to come in the future on the basis of the number of PCR positive cases recorded on a given day. The R2 number however, and Figures 4, 7, 8 and 9 , show that PCR positives do not correlate to excess deaths in the future. The implication is that PCR positives lack predictive power in terms of telling whether people will die in the future.
A possible explanation could be that the PCR positives simply measure the number of PCR tests taken on a given day, i.e. they might be somewhat proportional to the number of PCR taken on a given day, and positives might or might not be “infectious” positives. Ultimately, this means PCR positives cannot be used to tell if the pandemic is advancing if for that we understand that deaths are to increase or decrease. This agrees with the interpretation of CEBM above.
Finally, we want to point out that the same can be said for all countries we have examined, i.e. other than Spain. For example, in the months of July to September positive cases in Europe are said to have risen, but we find no evidence of excess deaths in the countries in Europe reported by euromomo.eu (Figure 10). We believe the rise in deaths toward August and September corresponds to the heat wave. It seems like this year the heat wave has been displaced toward August and September, rather than July and August as in previous years, in some European countries. In this work we have dedicated most attention to the Spanish data but more curves providing Positive PCR cases versus deaths (not excess but Covid19 as reported by each country) can be found at worldometers.info (https://www.worldometers.info/coronavirus/), John Hopkins, and other sources. Such data can be submitted to either visual inspection or PCR positive to excess death correlation as shown here. Our impression is that most data for all countries is in agreement with our interpretation, namely, PCR positives do not correlate to deaths in the future and are therefore meaningless, on their own, to interpret the spread of the virus in terms of potential deaths.
We suggest that the hypothesis of CEBM, i.e. that viral culture is required as a reference to test for infectivity, and other similar ones such as that by Jared Bullard et al[6]., i.e. search for relations between cycle threshold (Ct), symptom onset and infectivity in cell culture, should be explored in order to increase the predictive power of tests. Such predictive power is central provided the possible advance of the pandemic is to be understood and provided we understand that an advancing pandemic must be related to excess deaths in the future. Finally, regarding deaths, we must consider carefully Covid19 labelled deaths versus excess deaths. Covid19 labelled deaths depend on subjective parameters whether excess deaths have the advantage of being a standard relative to a reference, namely, the number of deaths in previous years. If we find many Covid19 deaths during a period but excess deaths are low or negative, it is likely that we are inflating Covid19 numbers. Furthermore, excess deaths typically depend on high/low temperatures, i.e. cold winters or heat waves (Figure10). Therefore, any light increase/decrease in deaths should be contrasted to the temperature. For example, heat waves might come in June, July, August or even September (2020 -Spain[7]) in Europe and direct comparison between years should consider this.
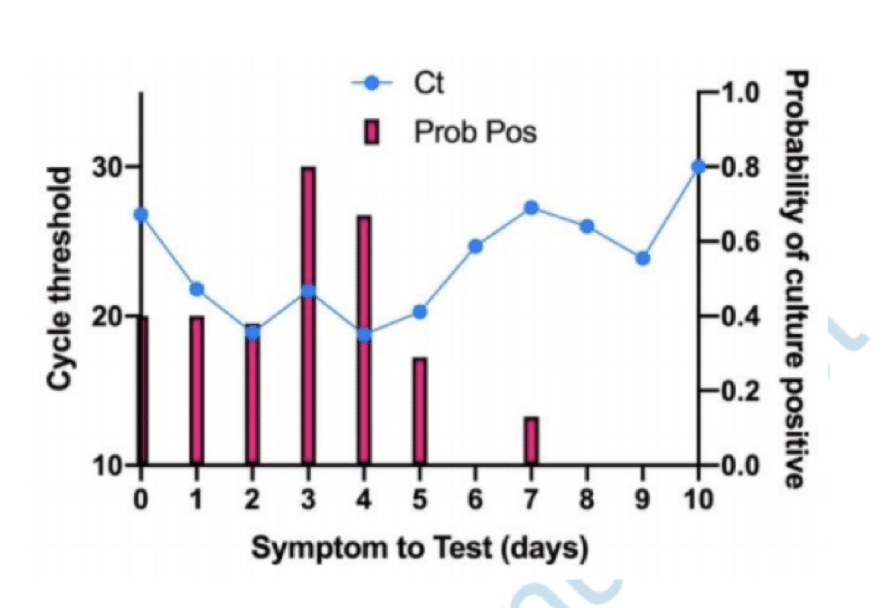
Figure 1. Time from symptom onset to RT-PCR, or symptoms to test (STT), was calculated based on laboratory records. The probability of successfully cultivating SARSCoV-2 on Vero cell culture compared to STT is demonstrated in Figure 3. The probability of obtaining a positive viral culture peaked on day 3 and decreased from that point.[6]
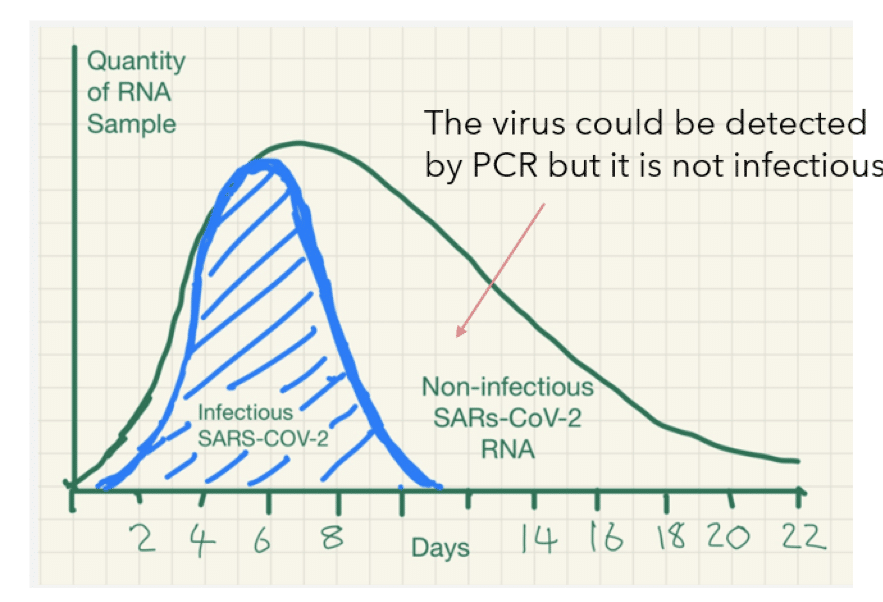
Figure 2. The shaded area shows that up to X days, i.e. 10 days approximately after infection, the virus is infectious. But then the virus is still present many days after. This could result in PCR positive but it does not mean that the virous is virulent or infectious, rather it means that residues and “non active” viral RNA is still detectable by PCR.
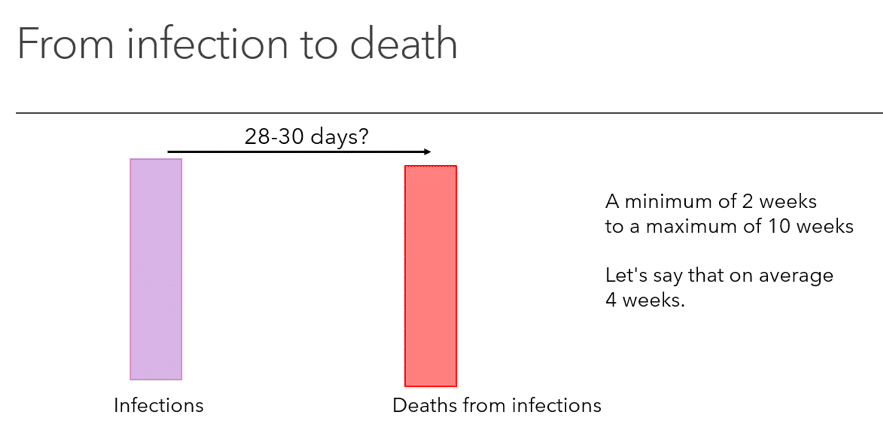
Figure 3. True infections today (PCR positives that are taken from a sample where the virus is still infectious or virulent) should lead to deaths in the future.
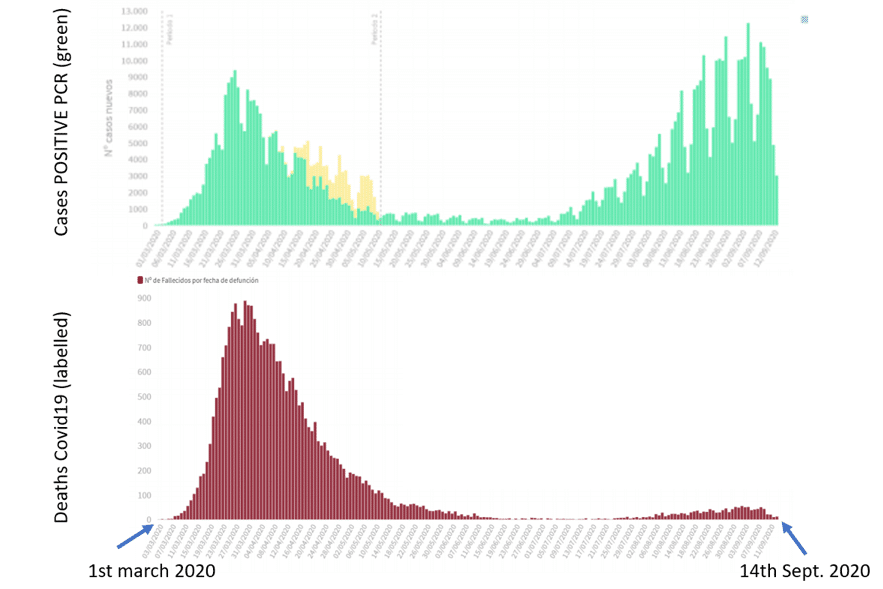
Figure 4. PCR positives in Spain (Top in green) versus deaths labelled as Covid19 deaths (Bottom brown) from march to the 14th of September in Spain according to the Ministry of health. https://www.mscbs.gob.es/profesionales/saludPublica/ccayes/alertasActual/nCov/documentos/Actualizacion_207_COVID-19.pdf
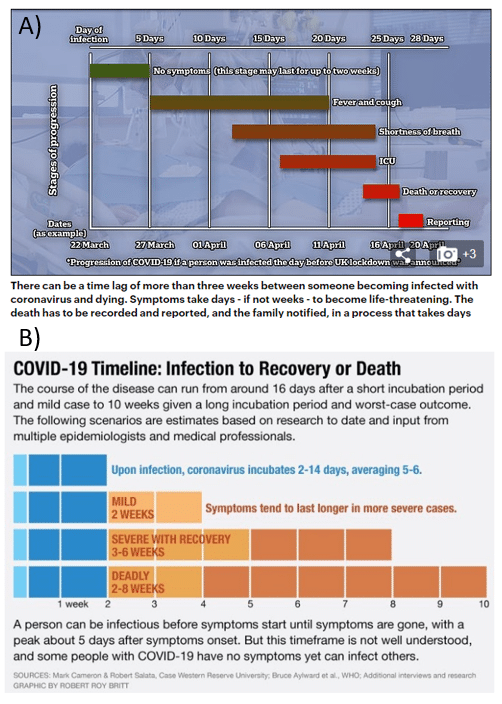
Figure 5. Time sequence from infection to recovery or death from difference sources as in a) 4 weeks approx. [8]and b) 2 to 8 weeks approx. [9]
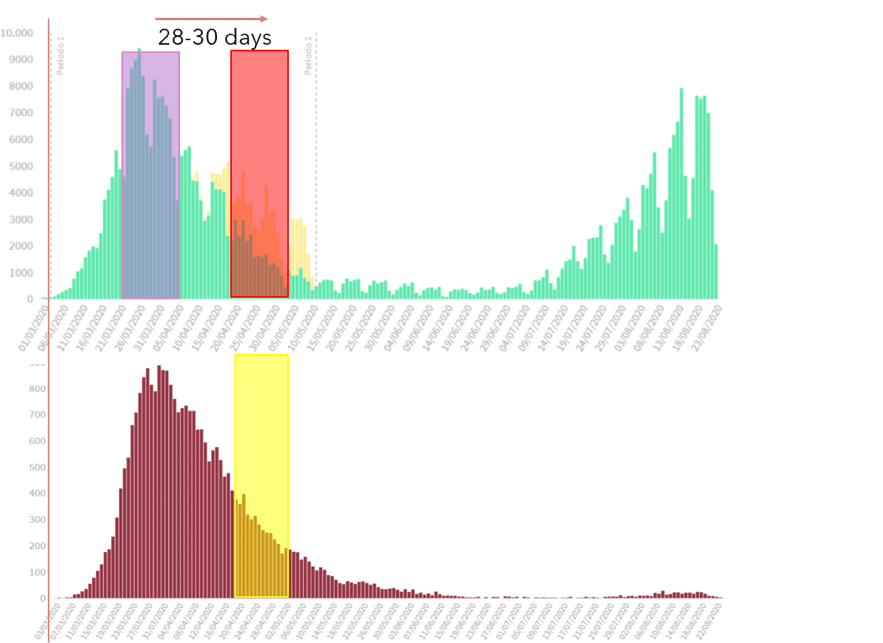
Figure 6. The peak in PCR positives in March-April in Spain (top green) does not lead to a peak in deaths 20-40 days later (bottom brown).
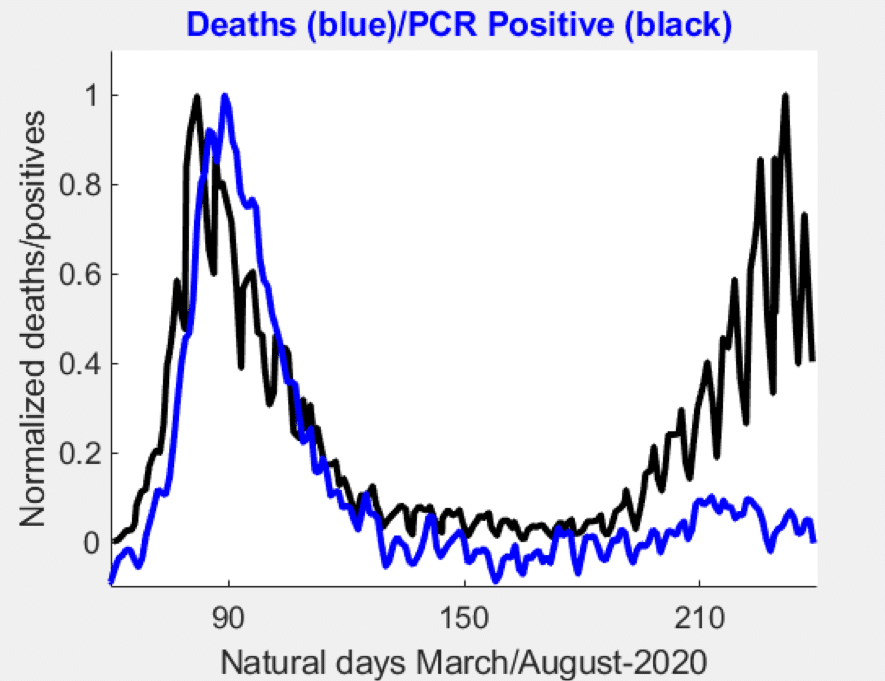
Figure 7. Normalized excess deaths in Spain (blue) against PCR positives (black).
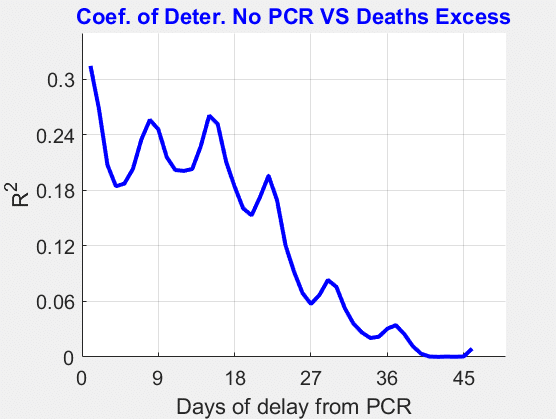
Figure 8. The x axis stands for the days of delay from the number of PCR positive recorded to the number of excess deaths. For example, if the X PCR positives were recorded today, 27 days of delay would mean that X is mapped to the excess deaths 27 days after the recording of the PCR positives. The y axis gives the coefficient of determination R2 as a function of days of delay. The highest values correspond to the proportionality between excess deaths “today” and “PCR positives today” implying that PCR tests lack any predictive power by being redundant at most.
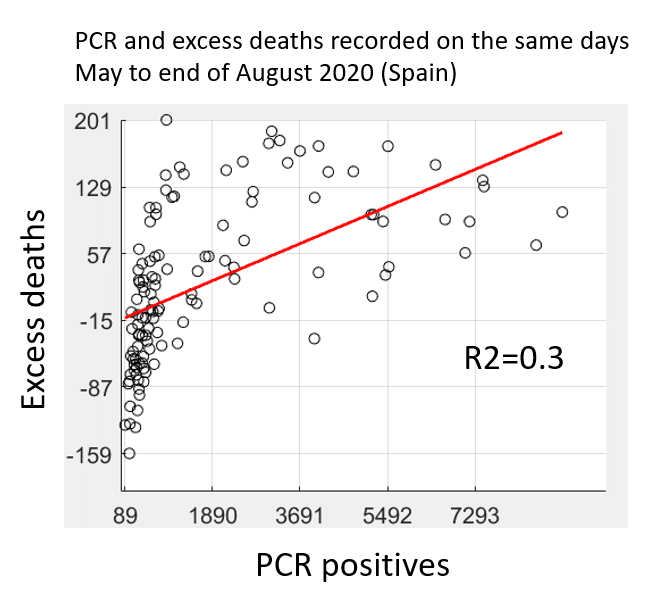
Figure 9. Scatter plot showing PCR positives versus excess deaths from may to the end of August. The coefficient of determination R2 is 0.3 and is highest when plotting the PCR positives recorded on the same day that excess deaths are recorded. The implication is that PCR positives have no “predictive power” since in this way they cannot predict if excess deaths will follow from PCR positives. As shown in Figure 8, the more delay we give to PCR in relation to excess deaths, the lower R2. A delay of at least a few days to weeks would be meaningful since governments could “expect” what is to come in the future on the basis of the number of PCR positive cases recorded. As shown the PCR positives do not correlate to excess deaths in the future and therefore lack predictive power.
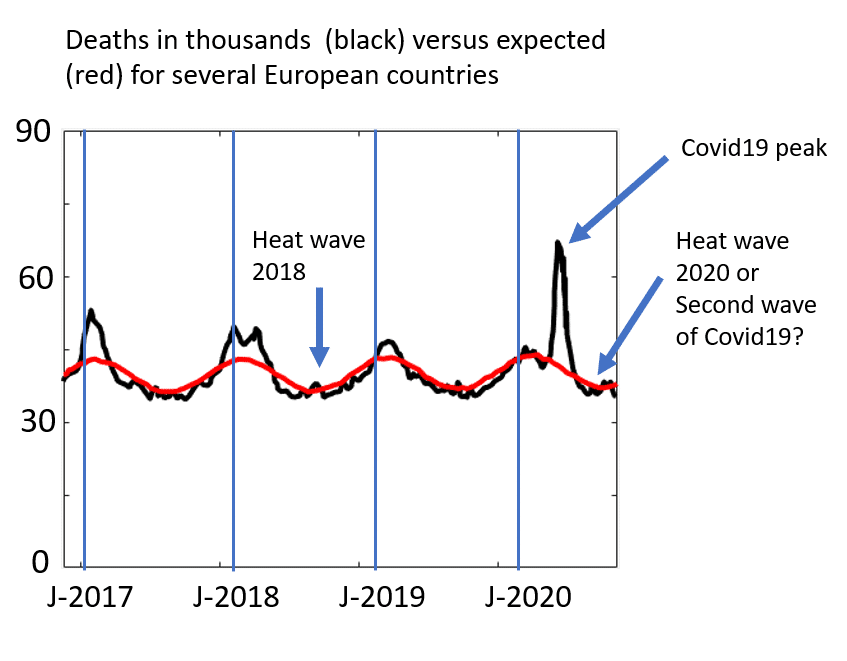
Figure 10. Deaths from 2017 to September of 2020 for several countries in Europe as recorded by euromomo.eu (https://www.euromomo.eu/graphs-and-maps/).
- Jefferson T, Heneghan C, Spencer E, Brassey J. Are you infectious if you have a positive PCR test result for COVID-19? In 5 August 2020 Edition. https://www.cebm.net/covid-19/infectious-positive-pcr-test-result-covid-19/: The Centre for Evidence-Based Medicine 2020.
- Jefferson T, Spencer E, Brassey J, Heneghan C. Viral cultures for COVID-19 infectivity assessment. Systematic review. medRxiv 2020; 2020.2008.2004.20167932.
- Diagnostics DC. SARS-CoV-2 Coronavirus Multiplex RT-qPCR Kit. In. https://www.creative-diagnostics.com/pdf/CD019RT.pdf: DC Creative Diagnostics 2020.
- BIOTEC C. Real Time PCR Detection Kits. In. https://www.certest.es/viasure/: Certest BIOTEC 2020.
- WHO. Estimating mortality from COVID-19. In. https://www.who.int/news-room/commentaries/detail/estimating-mortality-from-covid-19: who.int 2020.
- Bullard J, Dust K, Funk D et al. Predicting infectious SARS-CoV-2 from diagnostic samples. Clinical infectious diseases : an official publication of the Infectious Diseases Society of America 2020; ciaa638.
- tiempo.com. ¿Quién ha dicho que no puede haber una ola de calor en septiembre? In. https://www.tiempo.com/noticias/actualidad/ola-de-calor-septiembre-espana-cambio-climatico.html: tiempo.com 2020.
- Boyd C. The coronavirus death lag explained: How it can take three weeks between catching the disease and being hospitalised (and three days for the NHS to record the fatality). In. https://www.dailymail.co.uk/news/article-8192993/The-coronavirus-death-lag-explained-weeks-fatality-recorded.html: dailymail.com 2020.
- Britt RR. From Infection to Recovery: How Long It Lasts. In. https://elemental.medium.com/from-infection-to-recovery-how-long-it-lasts-199e266fd018: medium.com 2020.

