Differentiating viral from bacterial pneumonia
April 8, 2020

Carl Heneghan, Annette Pluddemann and Kamal R. Mahtani
On behalf of the Oxford COVID-19 Evidence Service Team
Centre for Evidence-Based Medicine, Nuffield Department of Primary Care Health Sciences
University of Oxford
Correspondence to carl.heneghan@phc.ox.ac.uk
VERDICT
A severe complication of COVID-19 is viral pneumonia. Distinguishing viral pneumonia from bacterial pneumonia is difficult in the community. In some cases, they could co-exist, increasing the chance of a more unfortunate outcome. However, there may be important clues in the history and the examination that can help differentiate the two. Recent guidance from NICE (UK) will support clinicians in this process.
BACKGROUND
Community-acquired pneumonia (CAP) can be caused by viruses, bacteria and fungi (Figure 1).
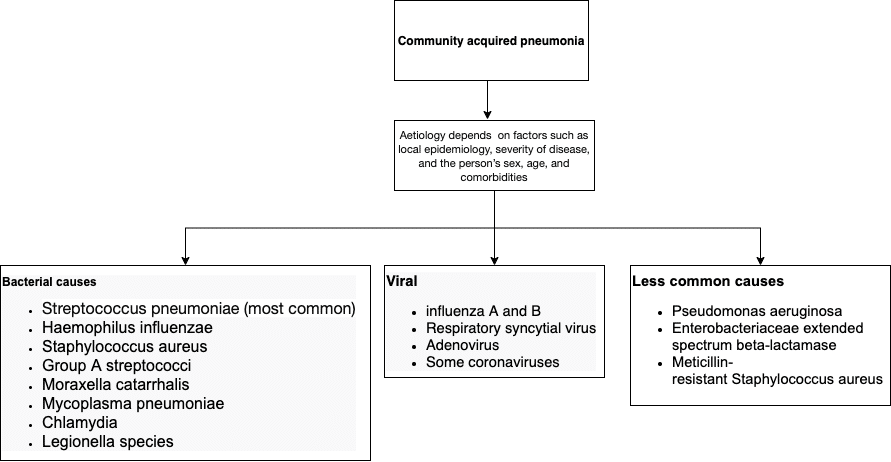
Viral pneumonia is a common complication of influenza-like illnesses and is a complication of SARS-COV-2. Viral pneumonia may clear up on its own; however, when severe, it can be life-threatening. Viruses are generally not as common a cause of CAP as some bacteria. However, as well as being a primary pathogen, viruses can be a co-pathogen with bacteria, particularly in those with severe illness requiring admission to ICU and in ventilator-associated pneumonia.
CURRENT EVIDENCE
Bacterial community-acquired pneumonia and viral pneumonia may coexist. A systematic review including 31 studies (n=10, 762 patients) found that 25% of patients with CAP had viral infections (95% CI 22–28%), this increased to 44% in studies where >50% had a lower respiratory sample. The review reported that the interaction of CAP and viral infection doubled mortality: odds of death in patients with bacterial and viral infection (OR 2.1, 95% CI 1.32 to 3.31) (10 studies).
Another systematic review of 28 studies (n= 8,777) identified respiratory viruses in 22% (95% CI: 18%-27%) of CAP patients, rising to 29% (25%-34%) in studies where polymerase chain reaction (PCR) detection was used. The review found that the proportion of mixed respiratory virus and bacterial co-infections in CAP patients was 10% (95% CI 6%-14%). Influenza (9%) viruses, rhinoviruses (5%) and coronaviruses (4%) accounted for the majority of the virus pathogens detected.
Coronavirus has also been shown to occur with CAP. In a 2010 case-control study conducted in Israel (n=183 adults with CAP, 450 controls), coronaviruses were identified in 24 (13%) patients with CAP, compared with 17 (4%) in control subjects.
Those more at risk include:
- The very young and the elderly (there is a decline in incidence from adolescence through to the fifth decade).
- Age-related immunosuppression
- Age-related comorbidities.
- Immunosuppressive therapy and secondary impaired immunities
- Disease-modifying heamatological/immunological agents in chronic illness
Differentiating viral and bacterial pneumonia
There are limited cues for differentiating bacterial and viral pneumonia.
In a cohort of 310 patients with viral or non-viral community-acquired pneumonia viral pneumonia was associated with:
- Rhinorrhea, multivariate (OR 3.52; 95% CI, 1.58-7.87)
- Higher lymphocyte fraction in the white blood cells,
- Lower serum creatinine,
- ground-glass opacity (GGO) in radiology results (multivariate OR 4.68; 95% CI, 2.48-8.89)
See also: Coronavirus Disease 2019 (COVID-19): A Systematic Review of Imaging Findings in 919 Patients..
The Development of a Bedside Predictive Model and Scoring System in 103 consecutive patients classified as having virus-like (48), bacterial (37) and unknown (18) pneumonia found that the independent predictors for bacterial pneumonia were:
- Acute onset of symptoms (OR 31; 95% CI, 6-150),
- Age > 65 or
- Comorbidity (OR 6.9; 95% CI, 2-23),
- Leukocytosis or leukopenia (OR 2; 95% CI, 0.6-7).
The sensitivity and specificity of the score to identify patients with bacterial pneumonia were 89% and 94%, respectively. The sample was small and the results might not be generalizable outside of the ED setting and they have not been validated.
A Diagnostic Rule for the Aetiology of Lower Respiratory Tract Infections in 145 adults [bacterial (n = 35), viral (n = 49), or dual infection (n = 8), or infection of unknown cause (n = 53)] found the independent predictors for bacterial infection were:
- Fever (OR 8.0, 95%CI, 0.9 to 71.0),
- Headache (OR 4.3; 95% CI, 1.0 to 19.1)
- Cervical painful lymph nodes (OR 8.7; 95% CI = 1.1 to 68.0)
- Diarrhoea (OR = 0.3; 95% CI = 0.1 to 1.0)
- Rhinitis (OR = 0.3; 95% CI = 0.1 to 0.9).
Procalcitonin
A meta-analysis included 12 studies of 2408 adult patients with documented bacterial versus non-bacterial aetiology of CAP. For the 8 studies using a procalcitonin cut-off of 0.5 µg/L, the pooled sensitivity and specificity estimates were 55% (95% CI, 37-71%) and 76% (95% CI, 62–86%), respectively. The review found that the sensitivity and specificity were both too low and variable for the results to be confidently used in the decision-making.
Supportive Care:
- Maintain oxygenation as needed.
- Maintain hydration either via supervised oral intake or intravenous fluids.
- Rest and decrease oxygen demand.
- Meet the increased calorie needs of the patient, secondary to the increased respiratory effort.
MANAGING SUSPECTED OR CONFIRMED PNEUMONIA IN ADULTS IN THE COMMUNITY DURING THE COVID-19 PANDEMIC
In the UK, the National Institute for Health and Care Excellence (NICE) has produced rapid guidelines for managing suspected or confirmed pneumonia in adults in the community during the COVID-19 pandemic. The guidance makes specific reference to differentiating viral COVID-19 pneumonia from bacterial pneumonia as follows:
| COVID‑19 viral pneumonia may be more likely if the patient: |
A bacterial cause of pneumonia may be more likely if the patient: |
- presents with a history of typical COVID‑19 symptoms for about a week
- has severe muscle pain (myalgia)
- has a loss of sense of smell (anosmia)
- is breathless but has no pleuritic pain
- has a history of exposure to known or suspected COVID‑19, such as a household or workplace contact.
|
- becomes rapidly unwell after only a few days of symptoms
- does not have a history of typical COVID‑19 symptoms
- has pleuritic pain
- has purulent sputum.
|
Expert opinion added suggestions include*
| Viral pneumonia more likely if |
Bacterial Pneumonia more likely if |
|
- Insidious onset
- Lower temperature
- Tachycardia or tachypnea out of proportion to the temperature
- A paucity of physical findings on pulmonary exam disproportionate to the level of disability
- Bilateral positive lung finding
|
- Acute onset
- Higher temperature
- Unilateral positive lung findings
|
|
|
|
|
|
*Viral Pneumonia. [Updated 2019 Dec 25]. StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513286/
If management can be maintained in the community, NICE goes on to suggest that:
- As COVID‑19 pneumonia is caused by a virus, antibiotics are ineffective.
- Do not offer an antibiotic for treatment or prevention of pneumonia if:
- COVID‑19 is likely to be the cause and
- symptoms are mild.
- Offer an oral antibiotic for the treatment of pneumonia in people who can or wish to be treated in the community if:
- the likely cause is bacterial or
- it is unclear whether the cause is bacterial or viral and symptoms are more concerning or
- they are at high risk of complications because, for example, they are older or frail, or have a pre-existing comorbidity such as immunosuppression or significant heart or lung disease (for example bronchiectasis or COPD), or have a history of severe illness following a previous lung infection.
- When starting antibiotic treatment, the first-choice oral antibiotic is:
- doxycycline 200 mg on the first day, then 100 mg once a day for 5 days in total (not in pregnancy)
- alternative: amoxicillin 500 mg 3 times a day for 5 days.
- Do not routinely use dual antibiotics.
- For the choice of antibiotics in penicillin allergy, pregnancy and more severe disease, or if atypical pathogens are likely, see the recommendations on the choice of antibiotic in the NICE antimicrobial prescribing guideline on community-acquired pneumonia.
- Start antibiotic treatment as soon as possible, taking into account any different methods needed to deliver medicines to patients during the COVID‑19 pandemic
- Do not routinely offer a corticosteroid * unless the patient has other conditions for which these are indicated, such as asthma or COPD.
- Safety net and review as appropriate
*Corticosteroids were widely used during the 2002-3 SARS outbreak. However, in a subsequent systematic review, including 29 low-quality studies of steroid use, reported on 25 studies that were inconclusive and four reported possible harm from steroid use. A further evidence review did not support corticosteroid treatment, reporting no evidence of net benefit with corticosteroids in “respiratory infection due to RSV, influenza, SARS-CoV, or MERS-CoV”, and that corticosteroids probably impair clearance of SARS-CoV.
CONCLUSIONS
Distinguishing viral pneumonia from bacterial pneumonia is difficult. There are important cues in history and the examination that can help differentiate the two. The clinician should be aware that the coexistence of viral and bacterial pneumonia increases the risk of death.
PUBMED LINK
We searched Pubmed using Clinical Queries Filters
systematic[sb] AND (viral pneumonia); (Diagnosis/Narrow[filter]) AND (viral pneumonia); (Clinical Prediction Guides/Narrow[filter]) AND (viral pneumonia), (Prognosis/Narrow[filter]) AND (viral pneumonia) and with the term COVID
End.
Disclaimer: The article has not been peer-reviewed; it should not replace individual clinical judgement and the sources cited should be checked. The views expressed in this commentary represent the views of the authors and not necessarily those of the host institution, the NHS, the NIHR, or the Department of Health and Social Care. The views are not a substitute for professional medical advice.
AUTHORS
 Carl Heneghan is the Editor in Chief BMJ EBM and Professor of EBM, Centre for Evidence-Based Medicine in the Nuffield Department of Primary Care Health Sciences, University of Oxford
Carl Heneghan is the Editor in Chief BMJ EBM and Professor of EBM, Centre for Evidence-Based Medicine in the Nuffield Department of Primary Care Health Sciences, University of Oxford
 Annette Pluddemann Course Director of the MSc in Evidence-Based Health Care and also a Senior Research Fellow in the Centre for Evidence-Based Medicine
Annette Pluddemann Course Director of the MSc in Evidence-Based Health Care and also a Senior Research Fellow in the Centre for Evidence-Based Medicine
 Kamal R. Mahtani is a GP, Associate Professor and Deputy Director of the Centre for Evidence-Based Medicine, Nuffield Department of Primary Care Health Sciences, University of Oxford. He is also an Associate Editor at the BMJ Evidence-Based Medicine journal and Director of The Evidence-based Healthcare MSc in Systematic Reviews
Kamal R. Mahtani is a GP, Associate Professor and Deputy Director of the Centre for Evidence-Based Medicine, Nuffield Department of Primary Care Health Sciences, University of Oxford. He is also an Associate Editor at the BMJ Evidence-Based Medicine journal and Director of The Evidence-based Healthcare MSc in Systematic Reviews

