What does RCGP surveillance tell us about COVID-19 in the community?
April 16, 2020
Carl Heneghan, Tom Jefferson
RCGP Surveillance Data: Updated 16 Nov
The RCGP surveillance data reports trends for Influenza-Like Illness (ILI), upper respiratory tract infections (URTIs) and lower respiratory tract infections (LRTI), along with weekly data on COVID-19 case investigations. The data comes from over 4 million patients in a network of general practices across England and Wales.
The figure shows that rates of confirmed Covid-19, URTIs and LRTIs rose in September. Rates of consultations for respiratory tract infections, however, are significantly lower than they were a year ago.
- In the week commencing the 11 Nov 2019, LRTI’s consults were 9.4 per 10,000 and URTI rates were 19.3 per 10,000 about four-fold higher than current consultation rates.
- Last year, rates of URTI consultations peaked in the week of the 16 Dec at 30 per 100,000 population and with LRTI rates of 14.7 per 10,000.
The current data suggest that Covid-19 consultations peaked around the week commencing the 19 Oct in primary care and are currently waning (there can be a delay in data though coming through that might change some of the estimates, particularly in the last 2 weeks).
The data also highlight that initial distancing measures, together with the seasonal effect, reduced transmission of URTIs by 9 per 10,000 (44%) in the week commencing the 9th of March (from 20 to 11 per 10,000 consultations). The following week (23rd March), when the lockdown was introduced, rates of URTIs further decreased by 3.3 per 10,000 consultations (29%).
Through Jan and February of this year, there were similar consultation rates of approximately 20 per 10,000 in Primary Care. These rates started to drop on the 15th of March. The trend in the data suggests that ARIs consult were displaced by COVID consults as shown in the figure below, with a peak in respiratory consults on the 15th of March.
There is a delay in reporting in the swab results that lead to fluctuations in the rates, particularly in the last week of reporting, but overall rates remain low. As more testing occurs you would expect more disease to be detected if it was circulating (see detection bias).
What we can say is there are low circulating levels of acute respiratory infections, lower respiratory infections and COVID-19 in the community that require consultations with general practice. The levels of suspected COVID-19 have not reached epidemic consultation levels and are dropping dramatically.
The RCGP surveillance has changed its outputs to confirmed, suspected or probable cases in the last week (see here). This has reduced the previously reported COVID-19 rates per 10,000 confirmed cases by about a factor of 10.
Do these rates constitute epidemic levels of community infection? Not at the moment.
An epidemic is declared if the rate of consultations for influenza-like symptoms in a sample of reporting by general practice exceeds 40 per 10,000 population in one week.
What does virology swabbing tell us?
Virology swabbing peaked in week 18 of 2020, The majority of samples remain for an unknown pathogen. COVID was first detected with viral swabs in week 9 (week ending 1st March) and peaked with 106 swabs in week 15.
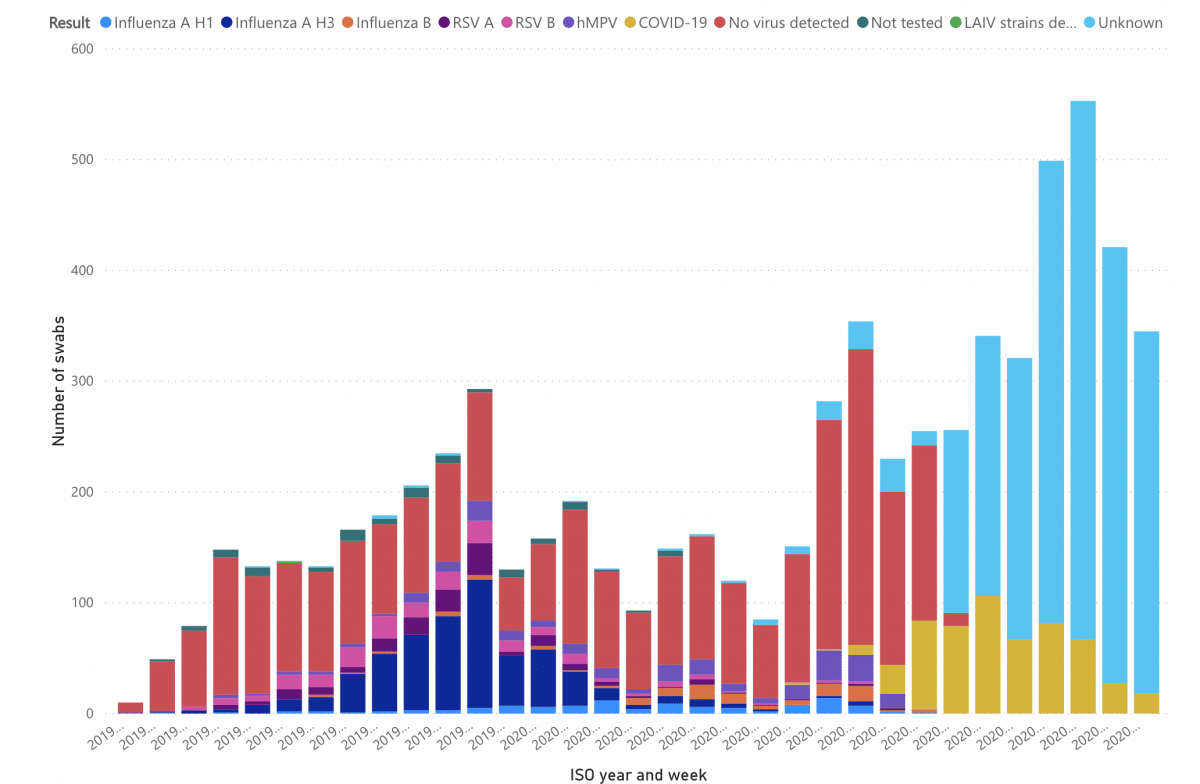
The explanations for these findings could be numerous: from contamination, to sample damage or unrecognised known agents, to looking for the most probable “culprits” (and not finding them). However, the presence of so many “unknowns” raises the possibility of the circulation of one or more co-agents.
This merits further investigation and explanation. Circulating unknown co-agents cannot be dismissed and should be thoroughly investigated as a matter of urgency. If found to be an artefact, it should be discounted for.
The simple observation also shows how useful a primary care sentinel network can be. If we want a quick fix to know what is going on, we should look no further than investing in such networks.
Research Surveillance Centre Data on COVID-19
 Tom Jefferson is an Epidemiologist.
Tom Jefferson is an Epidemiologist.
Disclosure statement is here

Carl Heneghan is Professor of Evidence-Based Medicine, Director of the Centre for Evidence-Based Medicine and Director of Studies for the Evidence-Based Health Care Programme. (Full bio and disclosure statement here)
The RCGP Surveillance Centre and CEBM is part of the Nuffield Department of Primary Care Health Sciences

