The increase in Deaths in the Home Setting: ONS Update:
August 18, 2020
Jason Oke, Carl Heneghan
The Office For National Statistics data on Registered deaths in England and Wales in the week ending the 7th of August 2020 (Week 32) showed there were 8,945 deaths. (152 mentioned COVID-19 on the certificate. 157 deaths fewer than the five-year average – the eighth week in a row that deaths have been below average.
The number of deaths in care homes and hospitals has been well below the five-year average, however, the number in private homes has been consistently above the average.
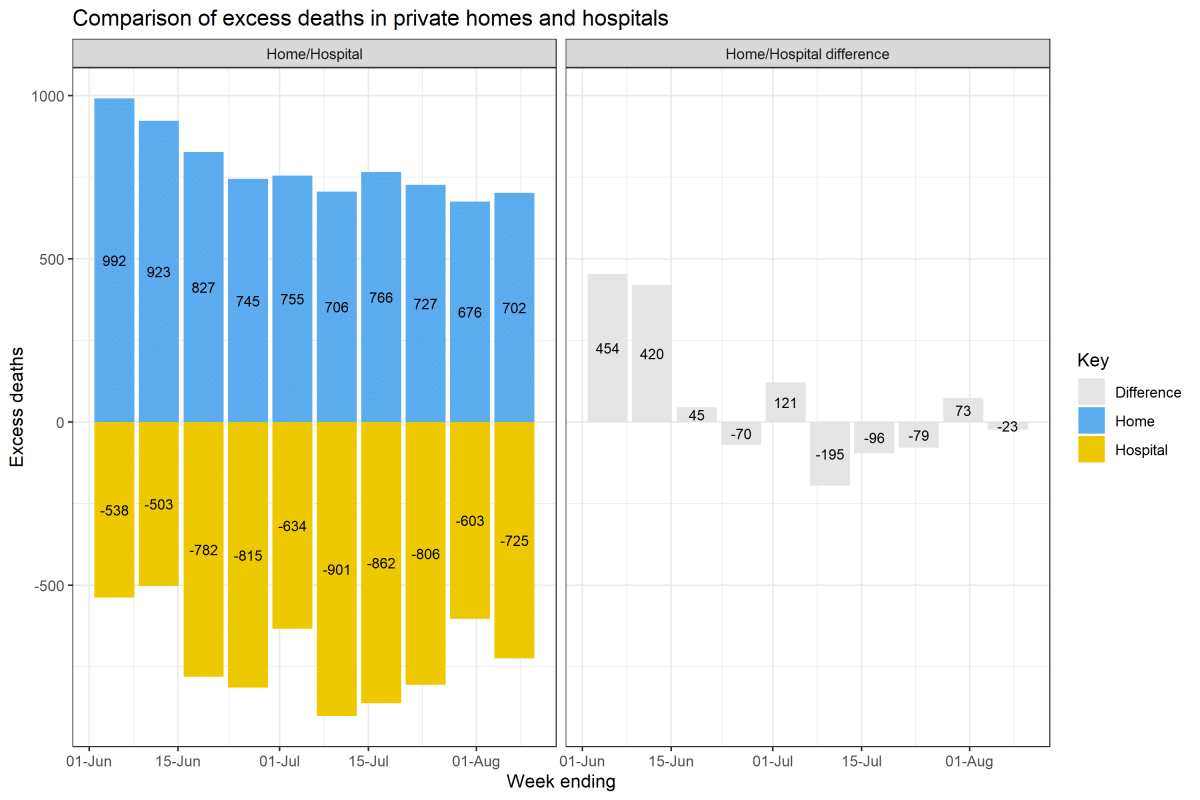
The figure shows there is a large excess in private home deaths over this period: 5,904 excess deaths over the 8 weeks (the blue bars). This excess is nearly cancelled out by the 6,108 fewer deaths (the yellow bars) occurring in hospital over the same time (the difference is 224 deaths).
This currently suggests the large excess in private home deaths is likely due to a shift in the place where people choose to die – away from hospital deaths.
A lack of resources in the community for palliative care might have meant previously that people often did not die where they wanted to. One factor that may contribute to this is the greatest fear expressed by many – dying in pain.
The 2014-15 House of Commons Health Committee, End of Life Care report, set out plans to enable people to die at home where that is their preference rather than in hospital. The ONS data suggests a significant number of people are now choosing to die in the home. Recognising this additional burden on community palliative resources is vital to ensure the move to dying at home is adequately resourced.
Jason Oke is a Senior Statistician at the Nuffield Department of Primary Care Health Sciences and Module Coordinator for Statistical Computing with R and Stata (EBHC Med Stats), and Introduction to Statistics for Health Care Research (EBHC), as part of the Evidence-Based Health Care Programme.
Carl Heneghan is Professor of Evidence-Based Medicine and Director of Studies for the Evidence-Based Health Care Programmes (Full bio and disclosure statement here).
Conflict: CH is a General Practioner and is an active NHS Urgent Care GP
Disclaimer: the article has not been peer-reviewed; it should not replace individual clinical judgement, and the sources cited should be checked. The views expressed in this commentary represent the views of the authors and not necessarily those of the host institution, the NHS, the NIHR, or the Department of Health and Social Care.

