Do weather conditions influence the transmission of the coronavirus (SARS-CoV-2)?
March 23, 2020

Jon Brassey, Carl Heneghan, Kamal R. Mahtani, Jeffrey K. Aronson
On behalf of the Oxford COVID-19 Evidence Service Team
Centre for Evidence-Based Medicine, Nuffield Department of Primary Care Health Sciences,
University of Oxford
Correspondence to jon.brassey@tripdatabase.com
Download: Weather conditions influence on the transmission of SARS-COV-2.pdf
Translated in Portuguese by Tatiane Bomfim Ribeiro, Rachel Riera, Oxford-Brazil EBM Alliance
22nd March 2020
VERDICT
Although much of the data has not been peer-reviewed yet, emerging evidence appears to suggest that weather conditions may influence the transmission of the novel coronavirus (SARS-CoV-2), with cold and dry conditions appearing to boost the spread. This phenomenon may manifest itself through two mechanisms: the stability of the virus and the effect of the weather on the host. The weather effect is minimal, and all estimates are subject to significant biases reinforcing the need for robust public health measures.
BACKGROUND
Most countries across the globe have now implemented a suite of strategies to reduce transmission of the novel coronavirus (2019-nCoV) and mitigate the effects of the COVID-19. The virus is known to have originated in the port city of Wuhan, in the central Hubei province, China. At the time when the first case was recognised, Wuhan was experiencing its winter season, where the average temperatures can range from 1 to 11 degrees Celsius. As of March 21st 2020, China experienced 81,008 registered cases of novel coronavirus with 3,255 deaths. However, for the first time, China is also reporting no new local cases. We conducted a rapid review of evidence to explore if climate conditions may influence the spread of (SARS-CoV-2.
CURRENT EVIDENCE
Studies exploring the effect of weather, mainly temperature and humidity, on the transmission of 2019-nCoV
A cross-sectional study correlated cases with mean temperature explored the effect of temperature on transmission in 429, mainly Chinese, cities. They found that for every 1℃ increase in the minimum temperature led to a decrease in the cumulative number of cases by 0.86.
A modelling study suggested a transitory reduction in incidence may occur cautioning “The onset of spring and summer could, for example, give the impression that SARS-CoV-2 has been successfully contained, only for infections to increase again in 2020-2021 winter season”.
Another modelling study found that the current spread suggests a preference for cool and dry conditions. They also report that the 2002-3 SARS-CoV outbreak was linked to similar climate conditions. If the COVID-19 pandemic follows SARS CoV-2 trends, then a worst-case scenario of a synchronous global pandemic would appear unlikely. The authors report that asynchronous seasonal global outbreaks were much likelier.
Analysis of the SARS outbreak in Hong Kong, Guangzhou, Beijing, and Taiyuan found the optimum environmental temperature associated with the SARS cases was between 16 to 28 degrees Celsius, which may encourage virus growth. A sharp rise or decrease in the environmental temperature related to the cold spell led to an increase of the SARS cases because of the possible influence of the weather on the human immune system. This study suggested a higher possibility for SARS to reoccur in spring than in autumn or winter.
It is important to note that all of these studies are potentially biased by uncontrolled confounding. Therefore, any conclusion has high uncertainty over their predictions. Other circulating viruses, such as influenza do follow a seasonal effect, and therefore co-infection rates will go down, which may impact on mortality. Assessment of exposures is prone to errors that can systematically distort the group-level exposure. For example, grouping cases by days of exposure may introduce a systemic error if the actual exposures for the case vary significantly or other measures were being introduced, i.e. isolation.
Two further studies report “daily mortality of COVID-19 is positively associated with diurnal temperature range (DTR) but negatively with relative humidity.”
Results suggest that temperature does positively correlate with infection rates spread, whereas it negatively correlates with humidity. Temperature and humidity are likely to contribute a maximum of 18% of the variation in transmission. Other variables, such as public health measures, account for the rest. A further investigation of air temperature and humidity influence on the transmission of (SARS-CoV-2) reported that for every 1℃ One increase in temperature and 1% increase in relative humidity lowered the R by 0.0383 and 0.0224, respectively.
Published 29th Feb, a modelling study produced the following figure to represent the relationship between temperature and the predicted the number of cases during the period of first reported case until 29th February 2020 (the grey zone represents the 95% confidence interval of the predicted values):
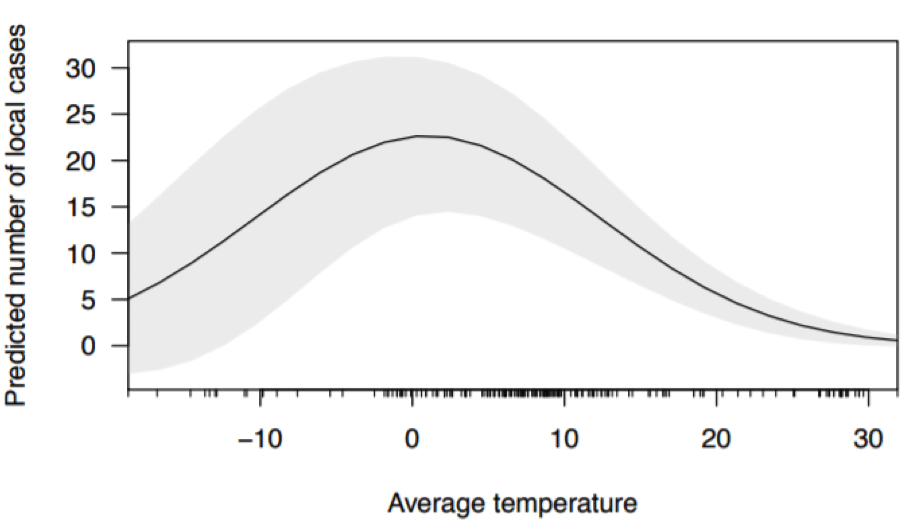
Not all of the studies we found suggested weather as an influence on transmission. An analysis of the reproductive number (R0) of (SARS-CoV-2) across China reported that changes in weather alone (i.e., increase of temperature and humidity) would not necessarily lead to declines in cases. The R0 across locations was calculated using incomplete reported case count data, with the date of reporting, rather than the date of onset used, which adds noise to any the estimation.
A further study on the role of Environmental Factors on Transmission Rates of the COVID-19 reports that the weather alone cannot explain the variability of the R0 in Chinese provinces, cities or other countries.
CONCLUSIONS
- Emerging data appears to suggest that cold and dry conditions may facilitate the spread of the novel coronavirus (2019-nCoV).
- However, caution is needed when considering the implications of these findings, which may be subject to confounding. In addition, much of the emerging data for 2019-nCoV has yet to be peer-reviewed.
- Although warmer climates may slow the spread of 2019-nCoV, relying on weather changes alone to slow the transmission of COVID-19 are unlikely to be sufficient.
Disclaimer: The article has not been peer-reviewed; it should not replace individual clinical judgement and the sources cited should be checked. The views expressed in this commentary represent the views of the authors and not necessarily those of the host institution, the NHS, the NIHR, or the Department of Health and Social Care. The views are not a substitute for professional medical advice.
AUTHORS
Jon Brassey is the Director of Trip Database Ltd, Lead for Knowledge Mobilisation at Public Health Wales (NHS) and an Associate Editor at the BMJ Evidence-Based Medicine
Carl Heneghan is Professor of Evidence-Based Medicine, Director of the Centre for Evidence-Based Medicine and Director of Studies for the Evidence-Based Health Care Programme. (Full bio and disclosure statement here)
Kamal R. Mahtani is a practising NHS GP, Associate Professor and Co-Director of the Centre for Evidence-Based Medicine, Nuffield Department of Primary Care Health Sciences, and Director of the MSc in EBHC Systematic Reviews.
Jeffrey K. Aronson is a physician and clinical pharmacologist working in the Centre for Evidence-Based Medicine in the Nuffield Department of Primary Care Health Sciences, University of Oxford. He is an Associate Editor of BMJ EBM and a President Emeritus of the British Pharmacological Society.
SEARCH TERMS
We searched the Google Scholar, PubMed and medRxiv using the following terms:
(Covid-19 OR SARS) AND (weather OR temperature OR humidity)

