The Ongoing Problem of UK Hospital Acquired Infections
October 30, 2020
Heneghan C, Howdon D, Oke J, Jefferson T
Probable Hospital Acquired infections in England remain persistently high: currently, 17.6% of COVID-19 infections fit the NHS England definition of probable healthcare-associated infections (HCAIs). These rates have been as high as 25% in the North West and continue to climb in the North East and Yorkshire.
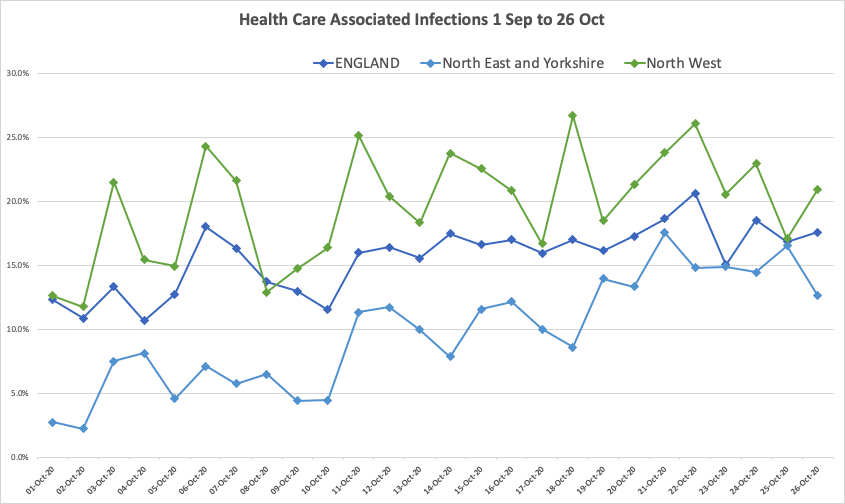
NHS England defines probable healthcare-associated COVID-19 inpatient infection as patients diagnosed more than 7 days after admission.
In terms of the number of hospital outbreaks reported by Public Health England in week 44 (between 19 and 25 October 2020), 71 incidents were reported where 59 had at least one linked case that tested positive for SARS-CoV-2. This result is stable compared with last week’s figure of 60 outbreaks.
We identified 11 news reports in October alone (see the table at the end of the article for the full details).
In Swansea there were 192 cases linked to hospital outbreaks, with 12 confirmed deaths linked to hospital infections in the Cwm Taf Morgannwg health board area, bringing the total so far to 69 at its three general hospitals in Llantrisant, Merthyr Tydfil and Bridgend. Overall, Cwm Taf Morgannwg health board has now reported 366 cases linked to outbreaks at the three general hospitals and community hospitals in Rhondda and Maesteg. Politicians have demanded a probe into outbreaks at the board’s hospitals, after 57 deaths related to outbreaks.
In Scotland, up to four people died after a Covid-19 outbreak on a cancer ward at an Edinburgh hospital.
In England, South Tees Hospital Trust has had seven separate outbreaks of Covid-19. An inquiry was launched in Tameside as in a small district hospital more than a third of all coronavirus deaths among inpatients in England occurred in a week. It has been found that 150 patients caught coronavirus in hospitals operated by University Hospitals Bristol and Weston Foundation Trust, of which a third died. This itself makes up almost a third of the total of 154 deaths in this trust over the course of the entire pandemic so far.
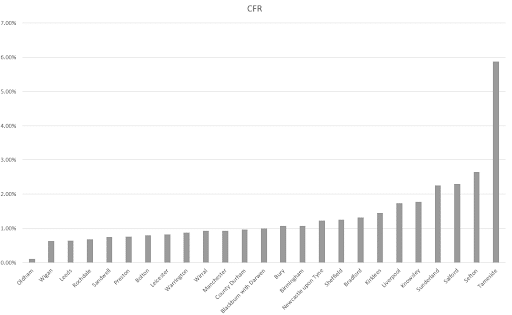
Although specific death rates linked to the Tameside outbreak are unavailable, we can assess the impact by applying a method previously used for estimation of the case fatality rate. Taking all areas in England with over 500 cases at risk for weeks 37-40, the case fatality rate in Tameside stands out as a clear outlier, with this value twice as high (or over three percentage points higher) than the local authority with the next highest death rate.
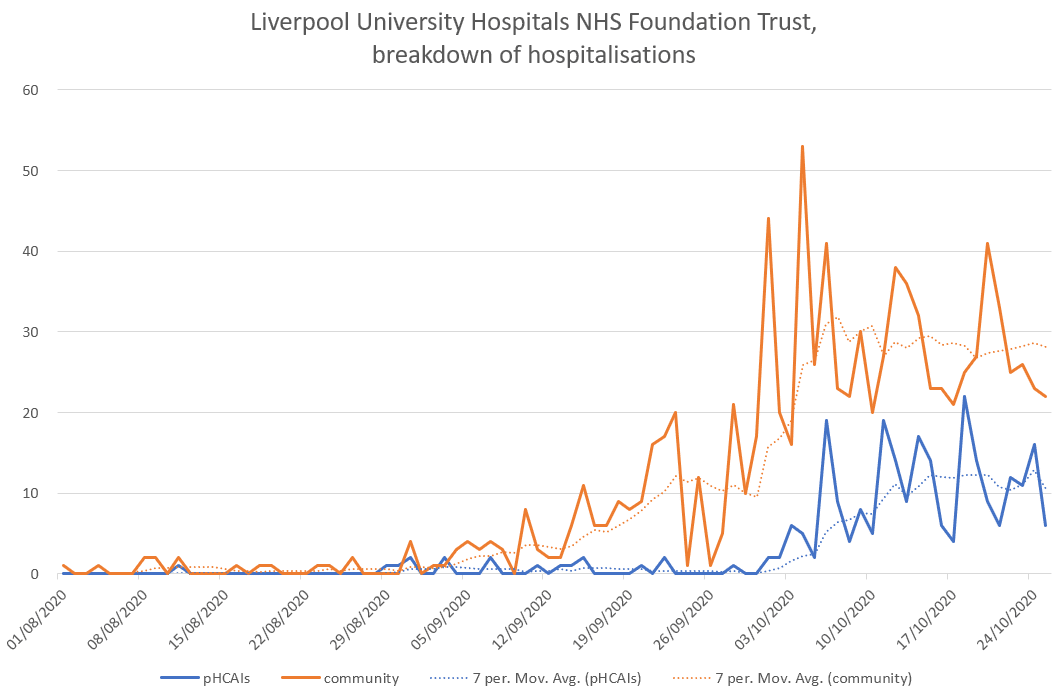
Liverpool University Hospitals NHS Foundation Trust has also exhibited a growing problem with probable HCAIs. While the trust continues to show persistently high total numbers of new patients in hospital with COVID-19 – a 7-day average of around 40 per day – admissions from the community have slowly fallen from a peak of around 31 per day on the 7th October. This general slow fall in community admissions has been masked in the aggregate, however, by an increase in probable HCAIs that began in early October, and peaked at around 13 per day in the most recent week of reporting. In the last week of reporting, probable HCAIs made up 27% of all new patients in hospital with COVID-19.
A study led by King’s College London estimated that at least one-eighth of COVID-19 hospital patients contracted the virus whilst already in hospital. The majority had already been in hospital for a long time. The study used a definition of hospital-acquired infection (HCAIs) occurring 15 days after admission with likely underestimation of the true numbers of HCAIs, which could be as high as 23%.
On 24 June, NHS England sent a letter requiring further action of all NHS Trusts and Foundation Trusts Strict application of the UK recommended Infection Prevention and Control Guidance was the main plan. This includes all staff in a hospital wearing a surgical face mask when not in personal protective equipment or in a part of the facility that is COVID-secure, and visitors and outpatients wearing a form of face covering. The guidance is set out here.
A rapid review in a large acute NHS Trust in South-West London identified 505 COVID-19-positive inpatients between 6 March and 12 April 12th. Forty-two (8.3%) tested positive >14 days after admission to hospital; 15 (3.0%) patients tested positive 8–14 days post-admission and had no compatible symptoms on admission. Highly probable and probable nosocomial cases were on average older (mean: 77.4 years) compared to community cases (mean: 67.7)
Table of News Stories on hospital-acquired infections
| 28 Oct |
Transmission of Covid-19 in Welsh hospitals reaches levels last seen in April
|
Over the week ending 25 October, there have been 192 cases linked to hospital outbreaks, with the largest number of new cases in Swansea Bay where numbers have more than doubled in a week to 59 “probable” and “definite” cases. ONS confirmed another 12 deaths linked to hospital infections in the Cwm Taf Morgannwg health board area, bringing the total so far to 69 at its three general hospitals in Llantrisant, Merthyr Tydfil and Bridgend. Overall, Cwm Taf Morgannwg health board has reported now 366 cases linked to outbreaks at the three general hospitals and community hospitals in Rhondda and Maesteg. |
| 28 Oct |
17 Greater Glasgow and Clyde hospital wards closed due to Covid outbreaks |
The health board reported 21 significant incidents of healthcare-acquired infections to Public Health Scotland. |
| 27 Oct |
COVID outbreak at Boston hospital closes three wards |
Three wards at Boston’s Pilgrim Hospital in Lincolnshire closed to new admissions following a series of COVID outbreaks. |
| 27 Oct |
Nottingham University Hospitals Trust NHS hospital forced to postpone cancer operations as Covid spreads on wards |
The prevalence of the virus has also meant staff and other patients in the hospital have become infected. As of Tuesday, the hospital was reporting 14 outbreaks on its wards which meant some wards being closed and other areas sealed off, further hampering its ability to provide services.
“Covid protected spaces for cancer services must be maintained to provide diagnosis and treatment safely, supported by frequent and fast Covid-19 testing of all staff – whether they have symptoms or not.’ |
| 22 Oct |
Three wards at Ninewells Hospital closed after Covid outbreaks |
NHS Tayside said it was investigating a “small number” of cases in Wards 2, 3, and 19. The three wards deal with gastroenterology, respiratory issues, and orthopaedics, respectively. |
| 21 Oct |
Hospital Covid infections rise in Wales by 50% in week |
The number of hospital Covid infections has risen across Wales by 50% in the past week. The party and the Welsh Conservatives have demanded a probe into outbreaks at the Cwm Taf health board, which has seen 57 deaths related to outbreaks. |
| 14 Oct |
A report on the numbers of outbreaks in the northeast and Yorkshire region, seen by The Independent |
70 separate Covid-19 outbreaks in hospitals and care homes on Monday” The report said South Tees Hospital Trust had seven separate outbreaks of Covid-19, with Newcastle upon Tyne Hospitals Trust and Tees, Esk and Wear Valley Trust each having six separate outbreaks. South Tyneside and Sunderland Trust had five outbreaks while hospitals in Sheffield, Leeds, Mid Yorkshire and Huddersfield all had at least four outbreaks on wards. Other hospitals in Doncaster, North Tees, Durham, Bradford and Barnsley had at least two separate outbreaks. |
| 13 Oct |
Coronavirus outbreak declared at another hospital in Wales. |
Swansea Bay health board said 10 patients and five staff had tested positive at Morriston Hospital in the past few days. |
| 12 Oct |
Covid outbreak at Newport’s Royal Gwent Hospital |
A coronavirus outbreak has been declared at Newport’s Royal Gwent Hospital. Aneurin Bevan University Health Board said 14 patients across three adult wards had been affected. |
| 9 Oct |
Several patients die amid Covid outbreak on cancer ward at Edinburgh hospital |
Up to four people have died after a Covid-19 outbreak on a cancer ward at an Edinburgh hospital, causing the department to be closed off as six more test positive. A multidisciplinary Incident Management Team was immediately established, and all necessary infection control measures are in place. |
| 6 Oct |
Covid outbreak at St Helier Hospital, South London |
Hospital has gone into partial lockdown while staff battle a Covid-19 outbreak that has infected seriously-ill patients in its intensive care unit and on a renal ward. A major investigation has been launched into how the infection got into patients being treated for other illnesses. |
| 15 Sep |
Tameside hospital fights fatal outbreak of hospital-acquired Covid |
Inquiry launched as several patients die of Covid-19 after becoming infected while being treated for other illnesses. A small district hospital where more than a third of all coronavirus deaths among inpatients in England occurred in a week. The incident is thought to be one of the first times the NHS has confirmed that an outbreak of hospital-acquired Covid has cost lives. – All 18 deaths are thought to have been elderly and to have had one or more underlying illnesses. |
| 10 Sep |
Weston general hospital in Somerset issues an apology |
An investigation found that Covid-19 may have contributed to the deaths of 18 people who contracted the infection during their treatment there. University Hospitals Bristol and Weston Trust admitted last month as many as 18 deaths could have been the direct result of contracting Covid-19 at Weston. 150 patients caught coronavirus at the BRI and Weston General Hospital – of which a third died |
Daniel Howdon is a Senior Research Fellow in Health Economics, Leeds Institute of Health Sciences. Bio here
Carl Heneghan is Professor of Evidence-Based Medicine, Director of the Centre for Evidence-Based Medicine and Director of Studies for the Evidence-Based Health Care Programme. (Full bio and disclosure statement here)
Jason Oke is a Senior Statistician at the Nuffield Department of Primary Care Health Sciences and Module Coordinator for Statistical Computing with R and Stata (EBHC Med Stats), and Introduction to Statistics for Health Care Research (EBHC), as part of the Evidence-Based Health Care Programme.
Tom Jefferson is an Epidemiologist. The disclosure statement is here.
Disclaimer: the article has not been peer-reviewed; it should not replace individual clinical judgement, and the sources cited should be checked. The views expressed in this commentary represent the views of the authors and not necessarily those of the host institution, the NHS, the NIHR, or the Department of Health and Social Care.Most viewed

